I do vitamin D levels on all my patients coming in for physical – they are almost always low. – Recently demonstrated that persistently low levels of Vitamin D associated with accelerated osteoarthritis and helping that helps. …
Am J Med. 2017 May 23. pii: S0002-9343(17)30506-5. doi:10.1016/j.amjmed.2017.04.038. [Epub ahead of print]
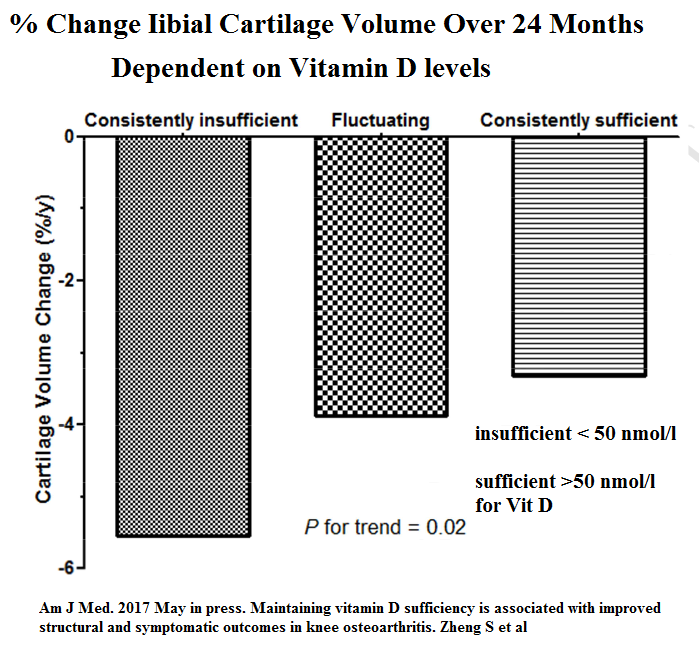
Maintaining vitamin D sufficiency is associated with improved structural and symptomatic outcomes in knee osteoarthritis.
Zheng S et al
https://www.ncbi.nlm.nih.gov/pubmed/28549923
- Study done in Australia – I’m not sure how they got ethics approval because I would not allow my patients to remain low on vitamin D.
- 413 cases mean age 63.2 years, 50% women
- took MRI’s to assess tibial cartilage size and Western Ontario and McMaster Universities Arthritis Index (WOMAC) for clinical status
Divided groups into
- Insufficient vitamin D = <50 nmol/l
- Sufficient Vitamin D + >50 nmol/l
- Fluctuating between 2 levels
Results:
There was no difference in pain and stiffness but functioning was down with stats p=0.04
This confirms a Framingham study finding that low Vitamin D associated with OA:
Low Vitamin D associated with Osteoarthritis
http://painmuse.org/?p=4013
addendum – also confirms an epidemiology study where dietary vit d consumption was analyzed:
J Nutr Gerontol Geriatr. 2017 May 30:1-13. in press
doi: 10.1080/21551197.2017.1317315.
Dietary and Supplemental Vitamin C and D on Symptom Severity and Physical
Function in Knee Osteoarthritis.
Hung M et al
https://www.ncbi.nlm.nih.gov/pubmed/28557644
“We found that supplementary vitamin D was strongly associated with lessened disability for knee OA patients.”
Comment – This makes 3 studies all associating low vitamin D with increase osteoarthritis knee issues. Over 2 years clinically there was not much difference but over a decade I could see this giving our patients a real problem. I check Vitamin D levels and they are usually low. There is little point in checking them as they will be low but it does not hit home to “invincible” patients that they are not right otherwise. Maybe knee OA concerns would. The word needs to get out there…