The common and disabiling pain condition is chronic lumbar radiculopathy (chronic back pain/Sciatica). Despite the widespread promotion of treatments of neuropathic pain a recent analysis of neuropathic pain treatments has concluded the following:
“To date, no medications have demonstrated efficacy in lumbosacral radiculopathy, which is probably the most common type of NP(neuropathic pain).” This was certainly a surprise to me.
Pain 132 (Dec. 2007) 237–251
Review and recommendations Pharmacologic management of neuropathic pain: Evidence-based recommendations Robert H. Dworkin et al
abstract here
This suggests a great need for potential agents. Local injections of Enbrel appears to be one of them with in some cases dramatic responses despite long term misery. This is one of the agents I fear our drug plan will never carry.
Conventional Treatments DO NOT work for leg pain radiculopathy.
After all this hype that Tricyclic Antidepressants should be tried first for Neuropathic pain, it was amazing that it worked so poorly for lumbar radiculopathy, the commonest of all neuropathic pains.
Initially, although a very small study, (6 patients on Nortriptyline) there was a suggestion of modest improvement of Nortriptyline,
Pain 76 (1998) 287–296
A placebo-controlled randomized clinical trial of nortriptyline for chronic low back pain
J. Hampton Atkinson et al
However, in 2007,a larger trial found Nortriptyline faired poorly with an average dose was 84 mg.; Morphine, tested separately, did poorly as well with an average does of 62 mg.
Pain 130 (2007) 66–75
Morphine, nortriptyline and their combination vs. placebo in patients with chronic lumbar root pain
Suzan Khoromi et al.
“In the 28 out of 61 patients who completed the study, none of the treatments produced significant reductions in average leg pain or other leg or back pain scores. Pain reduction, relative to placebo treatment was, 14% for nortriptyline (95% CI = [-2%, 30%]), 7% for morphine (95% CI = [-8%, 22%]), and 7% for the combination treatment (95% CI = [-4%, 18%]). Mean doses were: nortriptyline alone, 84 ± 24.44 (SD) mg/day; morphine alone, 62 ± 29 mg/day; and combination, morphine, 49 ± 27 mg/day plus nortriptyline, 55 mg ± 33.18 mg/day. Over half of the study completers reported some adverse effect with morphine, nortriptyline or their combination. Within the limitations of the modest sample size and high dropout rate, these results suggest that nortriptyline, morphine and their combination may have limited effectiveness in the treatment of chronic sciatica.”
The poor showing of morphine was not seen with fentanyl patch, where a 32% pain reduction was found in an “open label” study.
P.L. Dellemijn, H. van Duijn and J.A. Vanneste, Prolonged treatment with transdermal fentanyl in neuropathic pain, J Pain Symptom Manage 16 (1998), pp. 220–229.
Topiramate was found to work poorly for the leg pain but definitely helped the back:
Topiramate in Chronic Lumbar Radicular Pain
Suzan Khoromi,* Athos Patsalides,† Suzan Parada,‡ Vesta Salehi,*
Jennifer M. Meegan,* and Mitchell B. Max*
The Journal of Pain, Vol 6, No 12 (December), 2005: pp 829-836Abstract: Chronic lumbar radicular pain is the most common neuropathic pain syndrome. This was
a double-blind, randomized, 2-period crossover trial of topiramate (50 to 400 mg) and diphenhydramine
(6.25 to 50 mg) as active placebo to assess the efficacy of topiramate. Each period consisted of
a 4-week escalation, a 2-week maintenance at the highest tolerated dose, and a 2-week taper. Main
outcome was the mean daily leg pain score on a 0 to 10 scale during the maintenance period. Global
pain relief was assessed on a 6-level category scale. In the 29 of 42 patients who completed the study, topiramate reduced leg pain by a mean of 19% (P = .065). Global pain relief scores were significantly better on topiramate (P < .005). Mean doses were topiramate 200 mg and diphenhydramine 40 mg. We concluded that topiramate treatment might reduce chronic sciatica in some patients but causes frequent side effects and dropouts.
However side effects in study were bad:
“We would not recommend topiramate unless studies of alternative regimens showed a better therapeutic ratio.”
Pregabalin apparently failed in radiculopathy as well:
A.E.S.U. Remmers, L. LaMoreaux, J.P. Young, J. Moore and M. Poole,
Pregabalin treatment of patients with chronic low back pain (2000) Presented at the American Pain Society Annual Meeting, Atlanta, Georgia, November 2-5.
Another more recent larger study of pregabalin failed to find benefit in radiculopathy: see:
Sciatica Pain Is Different and Does NOT Respond Much to Pregabalin (Lyrica)
Given that Gabapentin is structurally very similar to Pregabalin, it is unlikely it would fare any better.
WHAT HOPE IS THERE FOR RADICULOPATHY?
A Enbrel pilot study in acute sciatica was spectacular:
Ann Rheum Dis. 2004 Sep;63(9):1120-3. Epub 2004 Apr 28. Efficacy of etanercept in the treatment of acute, severe sciatica: a pilot study. Genevay S, Stingelin S, Gabay C.
They used: “three subcutaneous injections of etanercept (25 mg every 3 days)”
“Results: In the etanercept group all variables improved: VASB from 36 to 7; VASL from 74 to 12; RMDQ from 17.8 to 5.8, and ODI from 75.4 to 17.3; all p<0.001. Pain (VASL and VASB: p<0.001) and ODI (p<0.05) were significantly better in the etanercept group than in the methylprednisolone group.”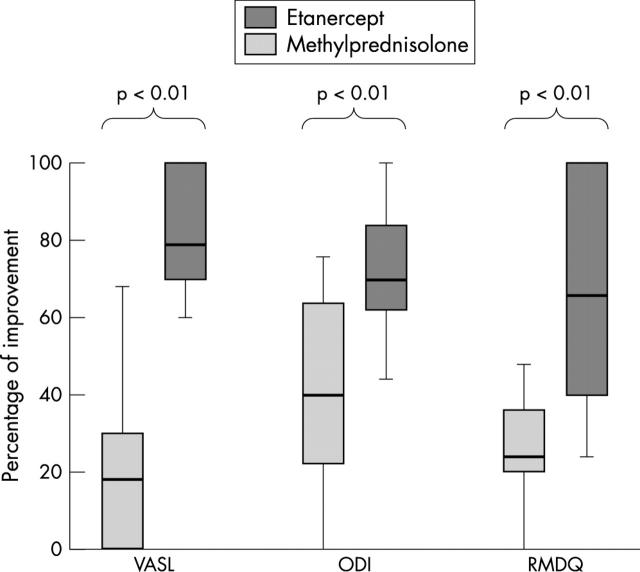
(from article above)
OK this is a busy slide;
The control group was given Methylprednisolone steroids.
VASL was the leg pains of sciatica
re VASL – The control group improved very little while the Etanercept improved 80-100%.
ODI was the Oswestry disability index, a commonly used disability score. It was significantly better in the Etanercept group and was the Roland Morris Disease Questionnaire(RMDQ), another disability measure.
Full article here
Another Pilot study, this time with hopeless chronic sciatica was :
Swiss Med Wkly. 2003 Mar 22;133(11-12):170-7. Perispinal TNF-alpha inhibition for discogenic pain Tobinick EL, Britschgi-Davoodifar S.full article here
Some of the results took my breath away. Here’s one:
“Case 4. Chronic discogenic pain; failed back surgery syndrome
This 57-year-old woman (patient 12, table 1) with a longstanding history of scoliosis treated by Harrington rod placement twenty years previously, presented for treatment of back pain and sciatica. For six years she had been experiencing constant and severe low back pain and sciatica unrelieved by three lumbar fusion surgeries. CT myelogram had revealed an extruded disk at the right L5–S1 foramen. Pain was present 24 hours per day, and both pain and numbness were experienced in the right lower back, right buttock, right thigh, right lower leg, and right foot. The patient also complained of weakness in the right leg and, to a
lesser extent, in the left leg. She was unable to walk for more than ten minutes, stand for more than ten
minutes or sit for more than fifteen minutes. Physical examination revealed intact deep tendon reflexes
in both knees, but absent achilles deep tendon reflexes bilaterally and decreased sensation in the right lateral foot. Straight leg raising was negative. Heel walking produced pain in the right lower back. Etanercept 25 mg by perispinal subcutaneous injection was administered to the lumbar region. Dramatic diminution in pain ensued within ten minutes. The patient reported 95% pain relief at one day post treatment. The Oswestry pain score prior to treatment was 60; at one month post-treatment it was 9, and at seven weeks continued to be 9. ”
This study required an average of 2.3 shots given a week apart. It was given paraspinously subcutaneously. At the time I wrote Tobinick about why it was not given as a nerve root – like block. His answer was “who are you?” as though my introduction in the letter was not enough. I did not send my CV as I didn’t think it was necessary and heard no more from him.
Intradiscal injection was not helpful:
Anesthesiology. 2007 Jul;107(1):99-105.
A double-blind, placebo-controlled, dose-response pilot study evaluating intradiscal etanercept in patients with chronic discogenic low back pain or lumbosacral radiculopathy Cohen SP, Wenzell D, Hurley RW, Kurihara C, Buckenmaier CC 3rd, Griffith S, Larkin TM, Dahl E, Morlando BJ
OH – did I mention they the failing disc study above gave only ONE shot despite the wisdom it takes an average of 2.3 shots. Initially, I tried giving just one shot enbrel to save costs; it did not work well. So an irritating shot directly in a disc only given once does not work – no surprise there.
addendum – a recent A pilot study on neck pain found good benefit:
Clin Ther. 2003 Apr;25(4):1211-8. Targeted etanercept for discogenic neck pain: uncontrolled, open-label results in two adults. Tobinick EL.
The more definitive study in chronic neck and back pain was done in 2004:
Curr Med Res Opin. 2004 Jul;20(7):1075-85. Efficacy of etanercept delivered by perispinal administration for chronic back and/or neck disc-related pain: a study of clinical observations in 143 patients.
Tobinick E, Davoodifar S. Institute Research Associates, A Medical Group, Inc, Los Angeles, CA, USA. etmd@ucla.edu
OBJECTIVE: Documentation of the clinical results obtained utilizing perispinal etanercept off-label for treatment-refractory back and neck pain in a clinical practice setting. RESEARCH DESIGN AND METHODS: The medical charts of all patients who were treated with etanercept for back or neck pain at a single private medical clinic in 2003 were reviewed retrospectively. Patients were treated if they had disc-related pain which was chronic, treatment-refractory, present every day for at least 8 h, and of moderate or severe intensity. Patients with active infection, demyelinating disease, uncontrolled diabetes, lymphoma or immunosuppression were excluded from treatment with etanercept. Etanercept 25 mg was administered by subcutaneous injection directly overlying the spine. Visual Analogue Scales (VAS, 0-10 cm) for intensity of pain, sensory disturbance, and weakness prior to and 20 min, 1 day, 1 week, 2 weeks, and 1 month after treatment were completed. Inclusion criteria for analysis required baseline and treatment VAS data. MAIN
OUTCOME MEASURES: Before and after treatment VAS comparisons for intensity of pain, sensory disturbance, and weakness. RESULTS: 143 charts out of 204 met the inclusion VAS criteria. The 143 patients had a mean age of 55.8 +/- 14, duration of pain of 9.8 +/- 11 years, and an initial Oswestry Disability Index of 42.8 +/- 18, with 83% having back pain, 61% sciatica, and 33% neck pain. 30% had previous spinal surgery, and 69% had previously received epidural steroid injections (mean 3.0 +/- 3). The patients received a mean of 2.3 +/- 0.7 doses of perispinal etanercept separated by a mean interval of 13.6 +/- 16.3 days. The mean VAS intensity of pain, sensory disturbance, and weakness were significantly reduced after perispinal etanercept at 20 min, 1 day, 1 week, 2 weeks, and 1 month with a p < 0.0001 at each time interval for the first dose in this patient population.
CONCLUSIONS: Perispinal etanercept is a new treatment modality which can lead to significant clinical improvement in selected patients with chronic, treatment-refractory disc-related pain. Generalizability of the present study results is limited by the open-label, uncontrolled methodology employed. Based on this and other accumulating recent studies, etanercept may be useful for both acute and chronic disc-related pain. Further study of this new treatment modality utilizing double-blind placebo controlled methodology is indicated. NOTE: This treatment method is protected by multiple patents awarded to Edward Tobinick MD, including U. S. patents 6 015 557; 6 177 077; 6 419 944; 6 537 549 and Australian patent 758 523.
The drug was not a panacea; It dropped Pain scores for 7/10 to 4.5 – 5/10 and persisted past 1 month + (length of study). On average, there was a 2 point drop in pain withing 20 minutes of being given.
The injection was given by perispinal administration as follows: “etanercept 25 mg was delivered to the soft tissue in anatomic proximity to the spine by subcutaneous administration utilizing a 23 gauge 1.5 cm needle directly overlying the midline of the back or neck, in accordance with the main area of symptomatology reported by the patient. ”
Please note it took an average of 2.3 shots to work. Also note some were epidural steroid failures, though I but maybe they were epidural steroid facilitators. By themselves, the steroid injections failed, but may have taken out some factors of inflammation not blocked by TNF inhibition. I had one lady who had epidural steroids one time and enbrel the next to tide her over to the time she could have her next epidural.
There was an initial study that demonstrated some benefit of infliximab IV infusion in scaitica.
Spine. 2003 Apr 15;28(8):750-3; discussion 753-4. Tumor necrosis factor-alpha monoclonal antibody, infliximab, used to manage severe sciatica. Karppinen J, Korhonen T, Malmivaara A, Paimela L, Kyllonen E, Lindgren KA, Rantanen P, Tervonen O, Niinimaki J, Seitsalo S, Hurri H.
Spine. 2003 Apr 15;28(8):750-3; discussion 753-4. Tumor necrosis factor-alpha monoclonal antibody, infliximab, used to manage severe sciatica. Karppinen J, Korhonen T, Malmivaara A, Paimela L, Kyllönen E, Lindgren KA, Rantanen P, Tervonen O, Niinimäki J, Seitsalo S, Hurri H. Department of Physical Medicine and Rehabilitation, Oulu University Hospital, Finland. jaro.karppinen@occuphealth.fi STUDY DESIGN: An open-label study was conducted. OBJECTIVE: To evaluate the efficacy and safety of infliximab, a monoclonal chimeric antibody, against tumor necrosis factor-alpha (TNFalpha) for the treatment of severe sciatica. SUMMARY OF BACKGROUND DATA: Evidence from animal studies indicates that TNFalpha plays a role in the pathophysiology of sciatica. Anti-TNFalpha therapy has not been previously evaluated in sciatic patients. METHODS: In this study, 10 patients with disc herniation-induced severe sciatica received infliximab (Remicade 3 mg/kg) intravenously over 2 hours. The outcome was assessed at 1 hour, 1 week, 2 weeks, 1 month, and 3 months after the infusion and compared to historical control subjects consisting of 62 patients who received saline in a trial of periradicular infiltration for sciatica. Leg pain was the primary outcome, with more than a 75% decrease from the baseline score constituting a painless state. Fisher’s exact test and repeated measures analysis of variance were used for statistical analysis. RESULTS: At 1 hour after the infusion, leg pain had decreased by 50%. At 2 weeks, 60% of the patients in the infliximab group were painless, as compared with 16% of the control patients (P = 0.006). The difference was sustained at 3 months (90% vs 46%; P = 0.014). Infliximab was superior over the whole follow-up period in terms of leg pain (P = 0.003) and back-related disability (P = 0.004). At 1 month, every patient in the infliximab group had returned to work, whereas 38% of the control subjects still were on sick leave (P = 0.02). None of the patients treated with infliximab underwent surgery during the follow-up period. No immediate or delayed adverse drug reactions and no adverse effects related to medication were observed. CONCLUSIONS: Anti-TNFalpha therapy is a promising treatment option for sciatica. There is an urgent need for a randomized controlled trial to evaluate whether these promising early results can be confirmed.
Another infliximab study on treatment of schmorl’s nodes (discs herniating into vertebral body) which found it needed to give four infliximab infusions. Their pain VAS scores went from 90/100 to 7/100 and from and 85/100 to 15-20/100. The former case completely cleared whereas the latter remained at 20/100
full article here
Now enter the MORON study:
This moron study has been used to refute use of TNF inhibitors:
Although all the prior studies with enbrel showed best results with regional injection of TNF inhibitors with average of 2.3 shots (first listed pilot study), and the above article with infliximab took four = 4 shots, some moron does a one shot IV study with infliximab (remicade). Earlier studies had showed 50% reduction of sciatica in the first day with remicade (above) but obviously one shot IV had no holding power.
Their one-shot not given locally but IV given study concluded:
“CONCLUSIONS: Although the long-term results of this randomized trial do not support the use of infliximab compared with placebo for lumbar radicular pain in patients with disc herniation-induced sciatica, further study in a subgroup of patients with L4-L5 or L3-L4 herniations, especially in the presence of Modic changes, appears to be warranted.”
My conclusions were that they should not let morons conduct studies. However, where ever I go to a conference this moron study is quoted because it was “randomonized and controlled” – they don’t mention it ignored all previous experience re requiring more than one shot.
I find Enbrel so helpful that at times I have paid out of my own pocket for a patient’s shot. Without the epidural steroid enhancements potentially in Tobinick’s studies, I find it will give me at least a 2-3/10 pain reduction lasting 3 months. For me, it takes 3-7 days to start working (depending how chronic) and takes TWO shots a week apart. I use a 27 guage long needle and give it paraspinously in the muslce on the side of the sciatica rather than midline. There is no need to go too deep as dispersion seems fast (some can feel it going up and down spine though I am not sure this is not placebo effect). Side effects I have seen have included one sore throat. The pharmacists like to give out enbrel preloaded syringes in groups of three – this is not necessary and don’t let anyone tell you they have to buy three. It will cost about $400.00 for two.
Warning: you can make a patient worse. The shots work and give the patient a false sense of being “cured”, though the pain will return by three months. At that point the patient will no longer be used to the pain. This will create a profound sense of despondency. Please set up a time-table and work out further shots in 10-12 weeks from the last one otherwise everyone is caught unawares.
I have an expression that fits many of my reactions to pain studies. It goes: “DIDN’T ANYONE BOTHER TO TURN OUT THE LIGHTS?”. People with radiculitis will have a large amount of myofascial accompaniment. Then there is the problem of “ceiling effect” – my take on that is that you can treat 9/10 problems a patient has and they will not necessarily feel any better because 1/10 problems can bring the pain to their ceiling of VAS-8/10. So just a plain enbrel shot may not give the results you are looking for. It will make it much easier to take out the quadratus lumborum/psoas and multifidi components, but they will still need lots of work. The leg triggers are often in piriformis, gluteal musclses, lateral calf, and posterior tibialis. They can be injected, needled and then respond to massage once the enbrel takes effect.
Very often one will find people with “myofascial pains” in shoulder, interscapular area, down arm, in buttocks and down leg. This will be associated with back or neck findings (restricted or painful movements). Since most big protrusions are gone after a years, the persistent radiculopathies are all just disc bulges, ignored by radiologists because many normals can have them. (This is so bad the bulges are NOT EVEN REPORTED; had a patient recently who had to get his specialist to specifically write that there was actually disc bulges not reported by radiologist). The problem is, CT/MRI’s cannot tell which ones are inflamed and inducing “chemical radiculitis” (discussed in another article). Some neck radiculitis cases showed positive response to nerve root block without evidence of foraminal problems at level injected. So how does one confirm radiculitis? I have found Enbrel response very useful for such and the patient is delighted by the relief of pain.
Addendum Nov. 2008 –
Joint Bone Spine. 2008 Nov 4. [Epub ahead of print] Antiepileptic drugs to treat pain in rheumatic conditions. Recommendations based on evidence-based review of the literature and expert opinion. Vergne-Salle P, Mejjad O, Javier RM, Maheu E, Fallut M, Glowinski J, Bertin P.
Reviewed evidence of help of epilepsy drugs in Chronic lumbar sciatica
1) Serpell MG, Neuropathic Pain Study Group. Gabapentin in neuropathic pain syndromes: a randomised, double-blind, placebo controlled trial.
Pain 2002;99:557-66. – “randomized, double-blind, placebo-controlled, 8-week study in 305 patients, among whom 21 had post-laminectomy sciatica and 27 a radiculopathy”
Pain dropped in the overall groups by 1.6/10, under the 2/10 required by some groups to be considered therapeutically significant. they make the point however that the decrease in pain scores do not reflect the increase in “social functioning and role emotional subscores” improvements.
Annoyingly, the majority of cases were NOT chronic radiculopathy, rather conditions like post herpetic neuralgia and CRPS which are totally different “creatures” than radiculopathy. Any benefits could be just from these cases. They also mentioned that ” 66% of patients had tried amitriptyline and 32% had tried antiepileptics” prior suggested not great responses either because they were a preselected poor responding group or because these agents are not that useful in first place.
I would be interested in other people’s experience or their comments. This is one of the articles to promote coverage of these agents by the drug plan.

I found your blog via Google while searching for back pain and leg numbness and your post regarding Etanercept (Enbrel) for Radiculitis (Sciatica) looks very interesting to me. I have seen many sites before and most of them do not look this good. I cannot wait to let my friends know about this site. Thanks for the excellent content.
I was astonished and frozen to the computer reading these results.
I am a nurse – 31 yrs. Have had disc bulge L4-5, L5-S1. Experienced extreme weakness to feeling of buckling legs. S/P 3 ESI’s, then fell. Surgery with lam and two level bilat foraminotomies.
1 yr P/O – dx chronic bilat radiculitis.
Some relief with meds. Very dificult to sleep. I would like to discuss
this possible tx plan with my pain specialist?
Dear Ms. Brockmann:
Your suffering brings up so many questions:
1) Leg weakness. My daughter and I presented a poster in Edmonton 2006 Canadian Pain Society on Commonly missed conditions in chronic pain. Among them were:
– B12 deficiency – a level under 200 would be a problem; it needs to be checked. If you are diabetic on metformin this can precipitate this problem even moreso.
– Low Vitamin D – a study in Calgary found that 100% of people not on supplements were deficient some time of the year. Low Vit D causes balance problems, and muscle weakness AND back problems:
Spine. 2003 Jan 15;28(2):177-9.
Vitamin D deficiency and chronic low back pain in Saudi Arabia.
Al Faraj S, Al Mutairi K.
http://www.ncbi.nlm.nih.gov/pubmed/12544936?dopt=Abstract
The above article found Vit d 10,000 units/day supplementation relieved back pain twice as often in cases with low Vit D than with those with normal Vitamin D levels. 25-Hydroxy Vitamin D levels can be done to check level. I use Osto – D2 50,000 IU one every 5-7 days to get effect.
– sciatica radiculitis will knot up multiple areas in the leg. The knots in the medial thigh adductors and quads are particularly associated with a buckling knee and need to be taken out. IMS (Intramuscular stimulation) can help achieve that. It has also been found to be helpful in neuropathic pain: (read free pdf of letter to editor)
http://www.pulsus.com/journals/toc.jsp?sCurrPg=journal&jnlKy=7&isuKy=782
A list of therapists can be found at the IMS website:
http://www.istop.org/
– Sleep disorders are common in chronic pain; opioid use is common as well. Both of those can cause low testosterone levels (yes, women make testosterone too and a free androgen index can be done to check it – I find they are often unmeasurable in women with chronic pain). Testosterone can improve muscle strength. I often put women with low testosterone on Andriol 40 one every other day.
– muscle weakness might be helped by rehab and you should see a rehab specialist.
– I do not belileve any entanercept or spinal steroid injections will help the weakness but if others have found elsewise I would like to hear about it.
– It has been suggested that sleep apnea can be precipitated by opioids. You might want to get a sleep study done. Two different Oxygen suppliers will do it – VitalAire will do overnight oxygen levels (oxymetry) for ~$75; Prairie oxygen will do that plus a nasal airflow study of ~ $170. I did a pilot oxymetry study and found frequent nocturnal oxygen desaturations common in chronic pain patients [hint – take any nail polish off…]
2) Bulging disc – this has to be the bane of chronic disc disease. – The repeated MRI disc followup studies by Jensen found that in persistent sciatica, the big discs often were better in a year but only 3% of the disc bulges got better. This would leave people with persistent sciatica from the irritating chemicals secreted by the disc, often without any evidence of the disc touching the nerve root. This is a new delineated entity called “chemical sciatica”. Both entanercept (TWO shots one week apart) and lumbar steroid epidurals might help that FOR THE SCIATICA – ie leg pains. Whether it helps back pain I’m not sure. People with foraminal stenosis may not respond well because certain movements will bang on the nerve root llike hitting a thumb with a hammer; no anti-inflammatory agent can compete with that… However with you foraminotomies this should be less likely. You can get the original article on Enbrel as I referenced in the above article – you could take that to your family doctor. It is a simple injection done with a 30 gauge needle into the interspinous ligaments. The steroid injections are done by the anesthetists and there are two in Regina that do them – Dr. Lang for one. I have more suggestions but that is all for now…
I found your blog via Google while searching for lower left side back pain and your post regarding Etanercept (Enbrel) for Radiculitis (Sciatica) looks very interesting to me. I just wanted to write to say that you have a great site and a wonderful resource for all to share.
Pingback: Pain Medical Musing » Blog Archive » Nerve Pain? - 21st Century Gene Therapy
Do you know or can you find out for me any pain management specialist in Pune India who will take time to study, diagnose properly and treat my left thigh radiculitis? Please try and let me know. Thanks.
I want to send this to my friends with similar problems how can I do it short of repeating the website address to them?
Excellent article I have been researching the use of TNF inhibitors for a few days now, due to my pain from a L5/S1 herniation. I have found studies dating back to early 2000 with Enbrel and Remicade and others that show promise. I have yet to find beside the INR in Los Angeles that do these injections consistently. I am in the process of preparing a portfolio of sorts to show my general practitioner why I NEED this treatment. If anyone who reads this knows of any doctor that is using this treatment in the chicagoland area, please let me know. Please accept my apologies Dr. Montbriand for using your forum in this way. I truly hope that with your forum more people can become aware of what you do. Thank you
I am very interested in the Enbrel treatment for chronic lumbar back pain but so far have been unable to find any practitioner in the New England area who knows about it and can do it for me. Even Chicagoland, as the previous poster requested, would be doable for me, since it is a short flight. If anyone knows anybody, please let me know andretonder@yahoo.com
Also, Dr. Montbriand, my apologies for using your forum in this way. And thank you for making available such an excellent resource.
Does anyone knows if Perispinal etanercept or similar is used in the UK?
People are asking what specialist can give enbrel shots. What people fail to notice is the shots are very easy.
What needs to be remembered is that the shots are subcutaeous – not really deep at all
“etanercept 25 mg was delivered to the soft tissue in anatomic proximity to the spine by subcutaneous administration utilizing a 23 gauge 1.5 cm needle directly overlying the midline of the back or neck, in accordance with the main area of symptomatology reported by the patient.“
I give the shot on the side effected at the level effected. The depth of the shot is no deeper than a hormone shot so any doctor could do it with their eyes closed… Any GP could easily do it… Don`t bother getting a specialist…
admin
regarding the perispinal enbrel shots, where can i purchase them and how affective are they based on having them done at inr’s clinic in LA?, is their procedure different or a different product?…i have called them a few times and they dont want to even tell me a rough price (even a ballpark worse case scenario with out paying a 300.00 usd over the phone consult) i live in BC, Canada and have exhaust every measure to treat this for 5 months and have had results but have pretty much baselined at one point and i dont want to get a surgery, although the endoscopic laser disc surgery does seem promising in india 3400-4500 usd!
any info would be helpful, thanks in advance
The shot is very simple and not much different than a buttock IM injection given for hormone shots etc. It could almost be given with your eyes closed:
Initial description” The injection was given by perispinal administration as follows: “etanercept 25 mg was delivered to the soft tissue in anatomic proximity to the spine by subcutaneous administration utilizing a 23 gauge 1.5 cm needle directly overlying the midline of the back or neck, in accordance with the main area of symptomatology reported by the patient. ”
Please note it took an average of 2.3 shots to work – given a week apart.
Your GP could easily give it.
Thank you for this information . I have siatica and plan on asking my doctor who is very openminded to give me these shots …Can he contact you if need be ?
Dear Wanda,
I have written these blogs to help doctors – he just has to read it re treatments of sciatica – the treatment is just a skin deep (although I go deeper) injection in back – the main concern is just the $400 dollars for the 2 weekly shots required…One has to have the brains to look for other causes as well – piriformis issues and iliocostal syndrome are two I have found in recent cases- – both written up in my site.
I printed this info and gave it to my doctor, he is quite happy to try this on me .Thank you
@Wanda…did u do it???and what were the results? i am in lots of pain and am interested in this treatment
I am really inspired together with your writing talents as well as with the structure in your weblog. Is this a paid topic or did you modify it yourself? Anyway stay up the nice quality writing, it is uncommon to see a nice blog like this one nowadays..
I had a unexpected fall and started having extreme pain in my low back region with redicular pain down the right leg to my foot, I tried steroid shots no help, had an MRI in which they found a Lesion 1.0×3.3cm in my right ilium crest with a fluid level, also a slight bulging at the L5 level, I had a bone scan done and there wass no uptake into the lesion, I had a second opinion done and they told me it was an aneurismal bone cyst and nothing to worry about, I went through physical therapy for 2 months, had facet injections and trigger point injections, nothing has helped, the butock region is very tight and the muscles ache with low back pain and redicular pain down the right leg, I also have a instability while walking on the right side leg wants to buckle at the hip area. 9 months has passed and I am starting to get left side stiffness and light pain down the left leg, I really dont know if there is something they missed on the mri, there was also a ct scan done to verify no fracture, nothing present, I am curious if anything can be done and if the lesion may be the cause of pain, What to do next, life is on hold for me????
for response see:
http://painmuse.org/?p=1597
sciatica really bad caused by a prolapsed disc, it has took me nearly three year to be nearly pain free but last week had a attack and now I’m back where I started three years ago. This treatment you have why is it not used buy all doctors, sounds too good to be true, is it available in the UK. I’m and in a lot of pain all the time, I have had physio the past, which help a bit, I have also had steroid injection in the spine which also help a bit, I would love too give this a try, the thought of this working and having a normal life would be a miracle. The past three years have cost me every thing, I was a carpenter which I can not do any more due to the pain, I am now in heavy debt due to not working much and am about to loose my home, I am in the middle of selling everything I own to survive and now it has cost me a 13 year relationship, I am not giving you a had luck story but just trying make you understand how much this can affect someones life. I am going to my GP next week and will ask her about this treatment, have you any more information about this in the UK if not please could you email me some information to give to my GP. Kind Regards Andy Turner
My mother has 2 herniated disc L4 L5 and the doctor says the nerve is compress by 70%. She is in a lot of pain. She is in bed all the time because of the pain. The doctor wants her to have a surgery. She is affraid.
Do you think etanercept will help?
The nerve that is pinched will stayed pinched without pain?? Is that right?
Thank you for your response.
Unfortunately, I find it impossible to give advice. I work on these patients:
Now initially I would offer daily B12 shots for 2 weeks – given by patients themselves as it can reduce pain 20-35% – probably not help someone tht severe though. A steroid epidural or selective nerve root block given pain specialist might be initial treatment. Etanercept would augment epidural if it failed to give enough relieve. For less severe cases I would:
1) Deal with painful quadratus lumborum/psoas – I pinch, from behind,around the back and get my fngers in front of quadratus lumborum. I pull it forward with my fingers until it releases some then I knuckle it until it comes out. If it is bad I inject the muscles much like a lumbar plexus block because I think these muscles might entrap these nerves some by their spasm.
2) Deal with any Maignes’ thoracolumbar problems by using an activator thumper/manipulator and massaging rotatories after by running fingers up and down until they let go.
3) Deal with any sacral areas by local/steroid injection by Blomberg techniques. Also deal with SI joints – a whole talk in self.
4) Deal with any medial back iliac crest points by injecting 5% lidocaine repeatedly to numb
5) Spend a great deal of time doing repeated transverse stretching to piriformis 15 – 20 min followed by knuckling out – a session up to 3 X week. Some cases have gluteal muscles involved and I would similarly treat though I would needle as well (gluteal ones often come out when thoracolumbar level treated).
6)When I was all finished these areas, it then became more apparent where the real pain was coming from – Last few severe cases I had, involved the lowermost rib rubbing on the ilac crest and irritating nerve on the ilaic crest mid laterally. There are actually 3 nerves that cross there laterally and so it is easy to get neuropathic level pain from far lateral – though they don’t feel it there until you take out some of the other areas. There should be 2 fingers between iliac crest and ribs and when the quadratus lumborum is bad, it drags it right down to nothing. When sleeping on side, bottom hip sags and uppermost ribs collide with iliac crst – same happens if they draw knees up at night – so if they complain sleeping make it worse – then wonder if it is this or a piriformis. It rubs when they walk and mimics spinal stenosis claudication (can’t walk more that 1-3 blocks due to increased pains)
7) If steroid epidurals don’t last long enough, , intrathecal midazolam might keep it under control. I find Enbrel works better in conjunction with steroid epidurals though have a couple that get 2 of them every few months or so.
8) There are cases I cannot help but are controlled on opioids and anti-neuropathic agents
So you can see, the decision for surgery comes from a lack of response to conventional therapies. Some, however, go straight to surgery depending on their unique circumstances that have to be decided on a case to case basis. I have one patient with bad pains and pressure on a nerve roots settle with work on piriformis and lateral ilac crest injections -as well as realizing that some of the pain was actually coming from the hip joint – either impingement or labral tear -waiting for dye enhanced MRI (doesn’t always show it though). Needlle/massage gluteal muscles posteriorly and Cyriax hip mobilizations gave temporary respites.
Of course ther are new innovations liked pulsed lower temperature radiofrequency to nerve spinal nerve ganglion at level which might help but I have no experience there. Ozone and botox injections have some benefits…
Good luck
I recently heard about a “new breakthrough in back pain relief” on the radio and called the number of the “Institute” in Boca Raton. They are asking almost $2000 for a nurse practitioner to do the injection and claim instant and long term relief. I found your site while doing some more research on this. I understand it is considered experimental by most insurance companies so they won’t approve it. Not having insurance anyway, I still want to know if I should spend the money with this place and if the procedure is effective at all, let alone long term. I have Fibromyalgia with the sciatica starting about 5 years ago. This was primarily on my right side and mild to moderate. About a month ago, it moved to my left side and has been excruciating to say the least. This was also accompanied by neck pain with radiating pain down my right arm including numbness and tingling. They say the epidural administration of Etanercept will help both conditions and relief can be instantaneous.
Can you tell me if they’re asking too much or if I should ask my current doctor if they can/will do it? Is this an effective treatment for both conditions? Any assistance would be appreciated.
I’m a 55 yr. old female with psoriatic arthritis, fibromyalgia and celiac disease. I am currently taking enbrel 50 mg. 2/wk, sub-q, for the psoriatic arthritis. I’ve suffered from herniated discs (L4-5 and L5-S1) and lower back pain for years. For the past year I’ve had excruciating sciatic nerve pain for which I’ve been give Lyrica, Gabapentin, local steroid shots in the buttocks, chiropractic treatment, TENS, pain creams, etc, etc. So when I learned about the spinal injections of enbrel as a treatment for sciatica, I contacted the Florida office of Dr. Tabinick and paid (thru the nose) for one treatment. Their claim is that one shot should do the trick, at the most 2. Well, my back pain went away for a day, range of motion increased and all my numbness and tingling disappeared. However, the nerve pain down my right leg didn’t feel any relief at all. It’s been a month since that first shot and all my back pain is back, as well as the numbness and tingling, too. My nerve pain is worse than ever and they want me to have a 2nd shot.
Their fee is $460 for initial consultation and $4000 for the shot, but when I said I didn’t have that, they immediatly dropped the price to $120 for the consult and $1250 for the shot, and if I wanted the 2nd one I have window of opportunity of 4 weeks at the reduced price, othewise it jumps to the $4000 original fee.
I did it because of the pain I am having, but I will not go for the 2nd one. The whole operation was very slick and I wasn’t comfortable with the evironment.
Question: I’ve been on IV/Remicade before, would it be a good idea to switch to Remicade again to see if it helps my back and nerve pain? Do you think it’s worth a try? I’ll go thru all the insurance changes and all that if I knew it’s worth trying. What do you think?
Miami, FL
Pingback: Enbrel Failure – So What Else Can You Do For Chronic Back Sciatica? | Pain Medical Musing
ive had severe sciatica pain for as long as i can remember. i live in canada. what do i have to do to get or an injection? (ie family doctor, specialist ). im in a desperate situation and have heard great things about this procedure
Family Dr. can easily give. I’m in Canada – let me know where you are from and maybe I can suggest someone.
I like this website and want to ask if these injections – PERISPINAL ETANERCEPT/ENBREL (are they the same?) are available in Australia/Melbourne?
I’ve been suffereing from sciatica for nearly 3 years, 57 years of age, had 4 epidural, had some relief but the last one did not work. Neurosergeon suggested operation. I have a feeling they don’t know eactly which nerves, they usually give me epidural between L4 and L5. There are also some pains in my neck and upper back – lately reflecting in the right arm. I was also on Lyrica which works for a few days and then you have to keep increasing dosage (like a real drug) and I stopped.
I suffere so much. Please help me with your answer.
Enbrel is used worldwide for arthritris and easily injected – usually required two shots a week apart. It lasts 10-12 weeks and is expensive.
I use midazolam when epidural steroid wear off
I have written a whole blog note of epidural/enbrel alternatives:
Enbrel Failure – So What Else Can You Do For Chronic Back Sciatica? at:
http://painmuse.org/?p=1891
COPPER TO TOUGHEN HERNIATED DISCS by Charles Weber
ABSTRACT Copper is part of lysyl oxidase, which is the enzyme that cross links elastin tissue. The strength of elastin depends on its cross links (Sandberg). Upper spinal discs are made of elastin. Therefore it is imperative that copper status be brought up to normal before an operation. Sometimes an operation will not even be necessary if this is done. Copper status must be kept normal thereafter in order to prevent a recurrence by total intake of at least 3 mg per day.
INTRODUCTION
Herniated discs are the most painful, and numerous diseases in modern society. Slipped or herniated discs are estimated to cost more than 200 billion dollars directly and indirectly each year in the USA alone [http://www.futuremedicine.com/doi/pdf/10.2217/14750708.4.1.51 ]. I suspect that copper deficiency status is the most important parameter affecting them. Two hundred and eighty patients having back pains were treated with copper salicylate. A majority was believed to have a slipped disc. Improvements were considerable and rapid [Sorenson & Hangarter]. Restoring copper during that disease is imperative.
Therefore increasing copper intake should have a dramatic effect on our collective health. Copper should always be made adequate even when a disc operation is in order. If the copper status is unknown, there should be at least a week of 6 mg total intake per day prior to the operation, or at least high in copper foods such as shellfish or liver, especially sheep liver. There should not be great danger if there is a concurrent bacterial infection because a depleted liver removes free copper from the blood with extreme rapidity, [Peisach, et al], so the danger of bacterial stimulation is probably not acute. Even so, using ceruloplasmin injections might be a safer way during such an infection because copper is tightly bound in ceruloplasmin.
CAUSES of COPPER DEFICIENCY
That copper is below optimum in a large number of people is virtually certain from current evidence. This is caused by the low copper content of dairy products, loss of copper by removal of the germ from grain, and refining of sugar. Fructose (corn syrup) and sucrose sugar in fruit apparently produces a much greater need for copper once in the body [Reiser] [Fields & Lewis]. Treating vegetables with the chelating agent, ethylene diamine tetraacetate, reduces both their copper and their zinc to 20% of original values [Pfeiffer, 1972,p161]. Eating large amounts of vitamin C (ascorbic acid or ascorbate) is thought to interfere with utilization of copper within the body [Harris 1991][Underwood p71] although Evans thinks the problem is that absorption is decreased [Evans 1973b]. Vitamin C does cause greater excretion of copper via the bile and decreased absorption [Van Den Berg], so these may be the main mechanisms for vitamin C’s interfering with copper. Vitamin C causes ruptures of the aorta in copper deficient animals [Owen]. Vitamin C inhibits copper sulfate injection to stimulate lysyl oxidase under a deficiency of copper if given before or at the same time as copper sulfate injection. But, strangely, if given 75 minutes later, accentuates copper’s affect in stimulating lysil oxidase [Di Silvestro, 1981].
WORLD COPPER STATUS
Polish people are said to average 30% below the RDR (recommended daily requirement) from food [Pietruska] and 70% of Japanese are below the MDR (minimum daily requirement) [Otsuki]. Keep in mind that the MDR is designated too low to start with, as is the RDR. Young adult American women average 1.16 mg per day [Murphy] and men about 1.5. The difference between the sexes is no doubt primarily due to women eating less food than men. People in Belgium average 1.5 +/- 0.4 mg per day [http://www.springerlink.com/content/m552011168630u37/ ]. Adolescent males, both incarcerated and free, are below the RDA [Gans] which has been set at 2.0 but should be at least 3.0. Porto Rican school lunches are below the federal RDR [Preston]. Hemodialysis patients have low copper and zinc serum levels [Komindr]. Even so, a full blown copper deficiency takes several months to develop in people with an injured digestive system, much longer than for zinc [http://www.nphp.gov.au/enhealth/council/pubs/pdf/copper.pdf (p68)]. This is because the liver stores large amounts of copper.
SYMPTOMS of COPPER DEFICIENCY
People vary considerably in their genetic makeup, and there are several dozen enzymes and hormones containing or affecting copper, so it should not be surprising that the symptoms of the copper deficiency diseases should vary greatly or that “spontaneous” remissions are possible. Other enzymes than lysyl oxidase require copper to activate them, They include; Two forms of Superoxide dismutase or SOD1 (Breaks down the superoxide free radical), Tyrosinase, Cytochrome c oxidase (Electron transport involved in energy production), Dopamine –hydroxylase, (Converts dopamine to norepinephrine), Clotting Factor IV (Blood clotting), Thio oxidase (Disulfide-bond formation), Protein Kinase (Development of Nervous System), Dopamine mono-oxygenase (Catecholamine Synthesis from Tyrosine), diamine oxidase,histaminase.
Low white blood cell count (neutropenia) is the earliest symptom in copper deficient babies [Cordano, et al]. The immune system is very sensitive to adequate copper [Prohaska & Lukaseqycz ][Percival]. TETA poison reduced IL-2 (interleukin-2) production 50% but not in the presence of copper supplements [Hopkins 1996] and interleukin-2 is reduced by a copper deficiency [Percival p1065]. Neutrophils are reduced in numbers as well as function and superoxide anion production is 60% less. 2.5 milligrams total per day prevented further decline but was not enough to return to normal even though neutrophils turnover every 3-5 days [Percival p1067]. Thus this is a reasonable basis for setting 2.5 milligrams as the minimum daily requirement. ). 2 mg per day is thought to be the minimum daily requirement (MDR) [Klevay 1982] and I suspect that 4 mg per day would be the safest intake (RDR) in order to cover everyone or perhaps the 6 mg. or so received in the Indies. Copper intestinal absorption is linear up to about 6 mg per day after which it tapers off (but based on rat experiments) [Marceau], so I would suspect that copper beyond about 6 mg would be superfluous. The standard hospital diet is less than 0.75 mg per day [Owen p13]. When you further consider that other nutrients and circumstances also vary enormously, at least for those eating processed food, it is not safe to assume that copper is not deficient because all the symptoms are not present. Any symptom should trigger consideration of increased intake from some source. Emphysema [Soskel], premature gray hair [Wu], blood clotting [Milne 1896], slow healing bone breaks [Dolwet], diabetes enhancement [Cohen 1982], high cholesterol [Klevay 1978] [Reiser] aneurisms, hemorrhoids [author’s observation], and anemia are such symptoms.
The median layer of the blood vessel (where the elastin is) is thinner from a deficiency but its elastin copper content is the same as normal men. The overall thickness is not different [Senapati, et al].
A copper deficiency halves serum DHEA (dehydroepiandrosterone) in rats [Klevay and Christoferson].
ELASTIN TISSUE
Elastin makes up the vertebrate disks above the sacroiliac, the blood vessels, much of the skin, the lungs, and the bronchial tubes of all vertebrates except the jawless fishes [Sage & Gray]. Elastin is about as flexible as a rubber band and can stretch to two times its length [Carnes 1977]. The 39 or more different kinds of collagen are about 1000 times stiffer. A healthy artery requires about 1000 mm of mercury or 10 times the normal mean blood pressure in order to rupture [Shadwick]. Therefore keeping strength of arteries up would seem to be even more important than keeping blood pressure down so far as arteries are concerned, although not necessarily so far as kidney glomeruli are concerned. However a copper deficiency coupled with high sodium (or high chloride?) causes disruption of the glomeruli basement membrane resulting in acute kidney failure [Moore]. Aneurisms are involved because copper is essential for lysyl oxidase, which enzyme cross links the elastin tissue. Numerous animal experiments have shown that a copper deficiency can cause diseases affected by elastin tissue strength [Harris]. The lysyl oxidase is secreted normally, but its activity is reduced [Kosonen] due, no doubt, to some of the initial enzyme molecules (apo-enzyme) failing to contain copper [Rucker] [Smith-Mungo]. Cross linking is especially crucial for elastin tissue because elastin gets all of its from cross linking [Carnes 1971] [Sandberg]. Elastin probably has a high turnover [Robert] and also may be porous to the enzyme, lysyl oxidase. I feel that improvement in less than a week is reasonable to expect for elastin tissue [Author’s experience]. Activation of lysyl oxidase itself is rapid in copper deficient chicks rising greatly 6 hours [Harris 1976]. Elastin has a fairly high turnover rate [Robert] and lysyl oxidase has a half-life of only 16 hours [Siegel]. Restoration of elastin is near normal by 3-4 days after copper has been restored in chicks [Tinker] so cross linking must be rapid even if turnover is not. However strengthening is hardly instantaneous. My own experience as a young man leads me to suspect one must allow at least a week for sure total strengthening of the whole tissue. A normal body contains about 100 mg of copper [Turnlund, 1998], so even someone containing only half of normal should be able to correct a deficiency in a reasonable time with a total intake no more than 10 mg per day (8 mg supplement or so for a junk food diet) because at least 30% should be absorbed, but cutting intake back to no more than 4 or 5 milligrams or so total [Osterberg 1980 pp. 135, 142] upon repletion and making sure that seven times as much zinc is taken with the supplement dose at least when a routine intake is established. I suspect it is preferable if the zinc is imbibed at a different meal than the copper. In animal experiments adequate intake may be 5 to 10 times as high as intakes which cause deficiencies [Klevay & Madeiros 1996 p2422S]. More than 6 mg per day routinely is said not to be effective because per cent absorption becomes very low after that amount [Wapnir 1998 p1055s][Turnlund & Keyes].
Milne found that 2.6 milligrams per day of copper could not recover a deficit in 40 days while 3 to 6 mg per day did it in about 30 days [Milne] so the recommended daily requirement should be at least 3.0 instead of the current 2.0. [Turnlund & Costa].
You may see an extensive review of the chemistry of lysyl oxidase and its action upon elastin and the 39 or more different types of collagen. [http://herkules.oulu.fi/isbn9514267397/isbn9514267397.pdf ]
COLLAGEN TISSUE
The strength of collagen is not as badly affected because of the long length of collagen molecules close order enabling hydrogen bonds to be affective. However inadequately cross linked collagen is subject to creep. The discs below the sacroiliac of the spine are composed of collagen. The strength of pig or chick tendon is little affected by copper deficiency, even though the animals are dying of ruptured aortas and even though the tendons have 70% the cross links of normal [O’Dell] [Chou]. The normal lesser number of cross links are desirable nevertheless, for they permit the tendons to return to their original position after stress is relieved and not to cold flow as polymers held together only by hydrogen bonds do. The number of cross-links is probably optimum, because too many would make the tendon brittle. Too few cross-links would cause the tendon to become slack with time. Thus the body has a tough material which approaches steel in strength weight for weight and bones which are almost as strong as cast iron (I do not know how cross linked bone collagen is although both bone and tendon are type I collagen [O’Dell]). The lesser reliance by tendon collagen on cross-linking for strength may be the reason why the body uses collagen to repair lesions in arteries during a copper deficiency instead of elastin [Waisman, et al]. Such a strategy may be a good immediate expedient for survival, but I suspect it results in an intractable hypertension eventually because collagen is much less rubbery or elastic than elastin. It is conceivable that something like that goes on to a lesser extent in spinal discs. It might be a good idea to find out
Ankylosing spondilitis probably heals slowly because the sacral and ileal joints are made of type I cartilage [Paquin, et al].
COPPER AFFECT on the SPINAL NERVE SHEATH and FLUID
A copper deficiency produces a degeneration of the spinal cord involving the sheath around the nerve fibers, It is similar to the degeneration caused by a vitamin B-12 deficiency. Winston and Jaiser have proposed that the similarity is because of a dysfunction of the methylation cycle, which is dependant on vitamin B-12 catalyzed enzymes and may be dependant on copper catalyzed enzymes also [Winston]. Methionine synthase requires copper and they suggest that s-adenosylhomocysteine may be regulated by copper.
There is raised copper in the cerebrospinal fluid during Parkinson’s disease [Beshgetoor]. Perhaps copper should be investigated for Parkinson’s disease.
MOVEMENT OF COPPER IN THE BODY
Copper, largely tied up as protein, enters the stomach, and there and in the upper intestine [Sachs, et al] [Underwood p70], the proteins other than those entering from the bile [Owen] are degraded (bile proteins are degraded in infant rats when glucocorticoids are low [Mistillis & Mearrick] ), thus making the bile the means of excretion for adults [Sarkar p246]. Loss in sweat is usually negligible [Underwood p74] as are losses in urine [Evans 1973b p547]. The copper is moved across cell walls possibly associated with certain amino acids [Neumann PZ & Silverberg M] [Sarka p236]. It may be alpha aminoisobuteric acid which is involved since this amino acid behaves the opposite of other amino acids from cortisol [Chambers, et al]. The copper is probably carried to a metallothionein barrier and storage substance by glutathione [Steinebach] and then moves past the metallothionein barrier inside the cells [Cohen, et al] into the serum. Both copper and zinc increase the metallothionein barrier [Oestreicher & Cousins]. The serum carries it, largely complexed to albumin and histidine [Frieden 1980 p104], to the liver. The liver rapidly [Peisach, et al p482] removes it and stores it until such time as unknown hormones (which probably do not include cortisol in any direct way) cause the liver to release ceruloplasmin (which protein contains copper) to bring copper to the target cells [Frieden] for general purposes, as well as unbound copper when under stress. The liver releases no copper to the plasma during a deficiency when the liver copper is below 2.7 milligrams per kilogram [Levenson 1998]. Adrenaline (epinephrine) stimulates ceruloplasmin release 150% [Weiner and Cousins] as well as free copper and may be the stress hormone for copper [Evans 1973b p556, 557]. Cortisol does not directly mobilize copper in stress. I suspect the immune peptide hormones (one or more of the interleukins) may be used to stimulate copper for immunity but I have no data. The ceruloplasmin transporter is destroyed by the target cells, which includes those that make bile proteins for copper excretion. Ceruloplasmin has a half-life of 130 hours [Sternlieb]. The target cells could include the cells that synthesize tropoelastin (elastin precursor). If these cells synthesize Lysyl oxidase (which cross-links connective tissue), they probably must incorporate the copper into that enzyme inside the cell [Harris, et al, p175]. Copper chaperone proteins move the copper inside the cell cytoplasm into target enzymes, which may be a process to avoid copper toxicity. These chaperones have been identified in cells from bacteria on up to humans. These chaperones and cell membrane transport proteins have been elucidated considerably in recent years, and are very complicated. A defect in the gene that makes ATP7A chaperone protein is responsible for causing Menkes syndrome and a defect in the gene responsible for ATP7B chaperone protein causes Wilson’s syndrome. Linder and Hazegh-Azam have written a review of copper movement inside the body [Linder].
Because anemia is the first clinical sign of copper deficiency, the goal of the study was to reduce ceruloplasmin to 20% of baseline value without reducing hematocrit below 80% of baseline. Brewer, et al [Brewer, et al] felt that ceruloplasmin is a reliable and sensitive measure of copper status at 20% and above, and tetrathiomolybdate was nontoxic when ceruloplasmin was reduced to 15-20% of baseline. However ceruloplasmin is not reliable when there is inflammation, infection or after surgery because ceruloplasmin makes up 80-90% of the blood’s copper or more. Ceruloplasmin content can be correlated with C-reactive protein (p69). C-reactive protein will rise 10 to 100 fold within 48 hours of infection or injury. Most of the enzyme systems other than growth factors were not degraded excessively. No exacerbation of toxicity was obvious by the addition of interferon alpha to the tetrathiomolybdate treatment in one of the patients. This procedure would probably work for other copper toxic conditions also, and was originally used to solve toxicity during Wilson’s syndrome. See this site for sources of tetrathiomolybdate, physician’s liability, and discussion with regard to Hodgkin’s syndrome. This may prove to be a good strategy to buy time until interferon, naltrexone, or other low side affect strategies can take hold (see discussion of naltrexone at the end). Supplements or copper rich foods should be used for babies with extreme care, as should be formula made from water out of copper plumbing (which can contribute 0.8 mg per day to adult intake [Delves HT]), or brass pots (which have harmed American Indian children [Bremner p45]), because babies can not excrete copper. Nursing babies would be even a little more at risk from supplements since mother’s milk contains five times cow’s milk [Delves p7]. Babies have 19 mg total copper at term, half in the liver [Klevay 1996 p2424] or more. New borne babies have 230 PPM (parts per million) in the liver, which compares to 35 PPM in an adult. It must be obvious that even 2 mg per day would overwhelm a baby in a short time if continued. Copper absorption is proportional to intake from breast milk and formula (in rats), which formula is up to 10 times the amount in breast milk [Lonnerdal 1998 p1048s], although babies can tolerate a fairly high oversupply of copper beyond the above (Lonnerdal 1998 p1051s], so they must have a mechanism for retarding absorption through the intestines during excess. Mason says that infants should get 0.05 milligrams/kilogram of body weight per day and premature infants should get 0.09 milligrams/100 Kcal [Mason p1998]. Cordano recommends between 0.42 and 0.135 milligrams [Cordano 1998]. That last may be too high.Two mg per day has been recommended for copper deficient babies, but I suspect this is much too high if maintained. Premature babies are usually born with too small a liver reserve to get safely past the nursing period, but one must use care with supplements. 0.09 mg per 100 Kcal has been recommended [Mason p2028]. I suspect that a seat of the pants criteria for such babies would be little more totally that is known to be absorbed from the particular source than the amount in the liver of normal babies above and beyond the amount they otherwise would receive in their mother’s milk. Perhaps half again as much would be reasonably safe. Normal should probably be two or three times as much per body weight as adults require or about 0.08 mg/Kg. and 0.04 for toddlers. Perhaps that ratio should be less for very fat babies. A full term baby has 230 milligrams per kilogram of liver of copper in its liver, or 105 mg per pound of liver [Dorea]. A full term baby goes from 2.5 milligrams to 9.5 milligrams total in its liver during the last 10-12 weeks of pregnancy [Cordano 1998]. I know of no reasonable way to determine clinically how much it actually contains although modern ultra sound devices should be able at least to determine liver size. Mason says that infants should get 0.05 mg/Kg per day and premature infants should get 0.09 mg/100 Kcal [Mason p1998]. I do not know at what age they can start to excrete copper. However they are said to have an adult like liver in two years [Evans 1973b] and their serum levels increase to near adult levels in one month (4-6 months for preterm babies) [Lonnerdal 1996]. All these problems of too much and too little are more arguments for using mother’s milk if at all possible. Babies are very important so it would be a good idea to throw as much light on problems of infancy as possible. we dare not give our babies just anything with no thought. We had better know as much as possible. A survey of infant formulas and ready to eat cereals disclosed that 25% contained no copper and non of the ready to eat cereal had copper or manganese even though half of them had more than 25% of the RDR for iron and zinc [Johnson]. They can not all have been correct. We would be wise to perform research to determine the best strategy as soon as possible.Of course it is essential that the mother receive sufficient copper before the baby is born. If she does not, birth defects can often materialize, which can persist into adult life. Fructose sugar, alcohol, silver, diarrhea, and diabetes can make the matter worse [Cordano 1998]. Older children probably are similar to adults in their handling of copper and should probably receive an amount about proportional to their weight (but I know of no long-term study). A 2.5-milligram per day supplement was given to a copper deficient child. It took 5 days for serum free copper to return to normal, 2 weeks for ceruloplasmin and neutrophils [Cordeno 1998].
COPPER STATUS TESTS
Red blood cell superoxide dismutase has been proposed as a good criterion of copper status in rats [Feller, et al]. However, blood cells maintain their copper as much as 15 weeks into a deficiency before dropping [Milne 1998]. Platelet cytochrome C oxidase is not sensitive to factors other than copper and blood platelet activity is said to be the most sensitive indicator [Milne 1996].
Plasma diamine oxidase has been proposed as a sensitive marker [Kehoe]. Plasma diamine oxidase (DAO) and liver content have been found to be the only way to distinguish between marginal and deficient copper states. However,
diamine oxidase is dependant on vitamin B-6, so it would not be a reliable indicator during a vitamine B-6 deficiency. The function of Diamine oxidase is the oxidative deaminating of several polyamines, essential substances for cell proliferation, which are found in rapidly proliferating tissues such a bone marrow and intestinal mucosa. DAO is thus a regulating enzyme to down regulate rapidly proliferating tissue and is important during pregnancy.
Liver biopsies are impractical but would be the best way if they were available [Klevay & Madeiros, 196, p2423S]. Kidney biopsies may prove to be just as indicative since their copper turnover is higher than liver (66% in the few weeks measured) [Levenson]. Brain and heart biopsies would be useless since their turnovers were 1% and 3% respectively [Levenson].
Hair analysis is ambiguous, does not change much [Danks p222][Hambridge], and subject to contamination. People with white hair have lower copper content than those with colored hair [Bertazzo] although old people will be often white haired even if their copper is adequate.
Marginal copper deficits do not change serum copper, or tissue copper-zinc superoxide dismutase enzyme even though ultra structural alterations in the heart, reduced copper in the brain, markedly decreased IL-2 production, and reduced immune function appear [Hopkins & Failla]. Serum contents of copper are not a reliable indicator since infections, emotional stress, and possibly potassium deficiency have an overriding effect. If the plasma free copper is less than 12 millionth of a mole, though, a deficiency is highly likely
There are many less lost time accidents in copper producing industries even though the number of accidents is greater [U.S. Department of Labor]. This would seem to indicate that copper miners are tougher than other miners, since each injury is less likely to cause lost time for copper miners. Also, the greater number of injuries to copper miners suggests that their greater toughness tends to make them more careless. I am convinced that this is because of copper’s role as part of the enzyme that cross links connective tissue. So, copper nutrition is important for anyone considering or preventing accidental injury or even treating it after the fact, including herniated discs.
Copper supplements would be infinitely superior to and safer than statin drugs [http://www.health-heart.org/causes.htm ] [http://www.thincs.org/unpublic.htm ] for lowering cholesterol or eating low cholesterol food [Couzin]. However adding copper without zinc can actually make that situation worse [Festa]. So if a patient is afflicted with high cholesterol it is apparently necessary to supplement with 7 times as much zinc the same day, but preferably at different meals. Copper is also essential for an adequate immune system [Prohaska 1981] [Percival]. Premature babies can have too little copper. However babies should be supplemented with extreme care because they can not excrete copper, which is excreted with the bile in adults. This care includes not making formula out of water from copper pipes.
CONCLUSIONS Copper deficiency is pervasive in our society because of very low copper content of dairy foods, refined grain and sugar, and honey. If copper is made normal by supplements or liver and shellfish for people with herniated discs, any operation will be sure to be more successful. In many cases an operation will even prove to be unnecessary if combined with an inclined bed in such a way as to stretch the spine.
REFERENCES [ http://charles_w.tripod.com/copper4.html ]. The articles starting at; http://charles_w.tripod.com/copper.html would be useful to you, especially copper from food in http://charles_w.tripod.com/copper3.html . There is also a copper and zinc table at; http://members.tripod.com/~charles_W/copperzinc.html expressed as weight per calorie, the most useful designation.
Would be nice if there was any Literature on Copper helping back pains or studies showing women with copper releasing IUD’s had less disc problems. I find it difficult to believe copper can be deficient in a society that passes its water through copper pipes. You need to do a study!
I have been suffering from a pinched nerve root which two MRIs have revealed is due to disc bulges at L5-S1. The pain is 24/7 numbness and tingling in both legs and feet as well as in hip area. I also feel inflamation in my lower back area which on some days gets worse and travels up the spine. Having tried multiple treatments none have lasting effect and relief. I live in Canada and would like to have a Enbral injection or Perispinal injection of Etanercept. My Family Doctor is not willing to give this injection. Can you please let me know where I can go for this injection in the Burlington/Oakville area or Greater Toronto or Hamilton areas? Thank you.
Etanercept/Enbrel was supposed to go generic but once word got out that it works in back pain, stroke, Alzhiemer’s and TBI better than anything else pig Pharma and their FDA lapdogs put a stop to it. Welcome to corporate run Nazi Amerika.
America is a filthy and evil country now.
——————-
From admin:
I have to admit, there is something inherently evil about the way they were able to extend their patent. I just hope some countries don’t buy it…
I am interested in finding out if the perispinal etanercept injections are available anywhere in the North East USA.
Pingback: Sciatica Pain Is Different and Does NOT Respond Much to Pregabalin (Lyrica) | Pain Medical Musing
Anyone in Melbourne doing this?
Can’t find any links
Please help
Anyone doing this in Melbourne ?
Please!
—————–
There is a major pain clinic in Melbourne…
If anyone has found out where a clinic or doctor will do the perispinal etanercept injection in Australia please contact me .
ph 0890721167
Hi Sue,
Just wondering how you got on, did you find anyone and did you get any relief?
Sigh…
Thank you for this information. It is giving me hope!
I have read your blog and all the responses top to bottom and I am not getting many leads on where I can get this done.
I know you said it is a very simple injection but it seems only the crooks in LA and Boca are willing to do the procedure. Furthermore, they claim that only one shot is needed.
I’m distrustful of these facilities and their astronomical cost. I am desperate to find an alternative and I am willing to travel, hell I’ll do the damn injections myself if I could get my hands on the drug.
I’m located in South Florida but like I said I am willing to travel.
If anyone has any leads please contact me at edd.laura.h@gmail.com
Thank you!