Dr. AV Apkarian has pioneered the idea that brain changes occur following pain injury that leaves a pain memory.
Mansour, A. R., M. A. Farmer, M. N. Baliki, and A. Vania Apkarian. “Chronic pain: the role of learning and brain plasticity.” Restorative neurology and neuroscience 32, no. 1 (2014): 129-139.
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4922795/
“We argue that the definition of chronic pain can be recast, within the associative learning and valuation concept, as an inability to extinguish the associated memory trace”
Perhaps early use of steroids can prevent this pain memory as seen in whiplash and more recently, in a PTSD like situation.
With the idea pain is a memory engram, loosing one’s memory can result in pain relief:
Choi, Daniel S., et al. “Sudden amnesia resulting in pain relief: the relationship between memory and pain.” Pain 132.1-2 (2007): 206-210.
https://www.sciencedirect.com/science/article/pii/S0304395907003491
Chronic Whiplash injury appears to be prevented some by methylprednisolone/steroid:
Pettersson, Kurt, and Göran Toolanen. “High-dose methylprednisolone prevents extensive sick leave after whiplash injury: a prospective, randomized, double-blind study.” Spine 23.9 (1998): 984-989.
- dose same as used in spinal cord injury study which was:
- 30 mg/kg bolus and 5.4 mg/kg/hr for 23 hours
- this is a huge dose: for 70 kg person is 2.1 gm initially and then 378 mg/hr x 23 hours = 8700 mg over 23 hours.
It cut whiplash pain incidence in near half after 6 months:
2.5/10 + 4/10 +5/10 three out of twenty pain cases and severity in methylprednisolone group
6.5 + 6 + 5.5 + 3 + 3 /10 – five out of twenty cases
Sick leave before and after was significantly better in treated group (busy pic):
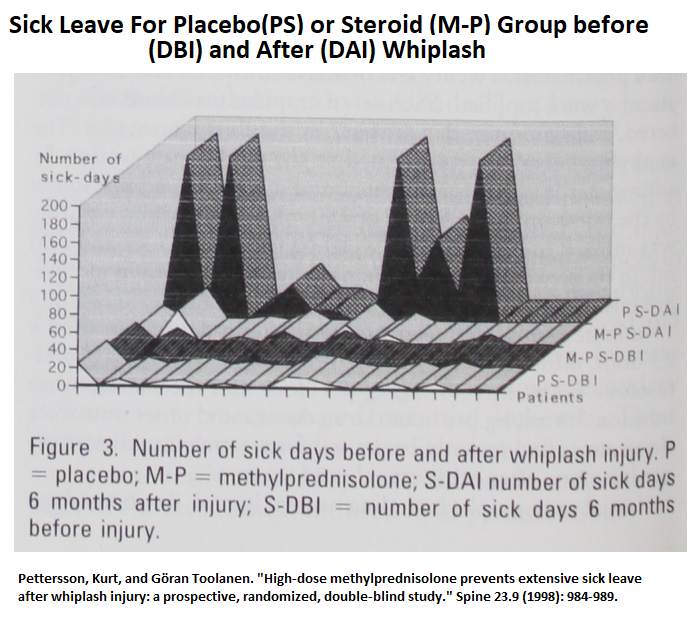 “At the follow-up examination 6 months after initial treatment, there was a significant difference in disabling symptoms between the actively treated patients and the placebo group (P = 0.047), total number of sick days (P = 0.01), and sick-leave profile (P = 0.003)”
“At the follow-up examination 6 months after initial treatment, there was a significant difference in disabling symptoms between the actively treated patients and the placebo group (P = 0.047), total number of sick days (P = 0.01), and sick-leave profile (P = 0.003)”
The numbers were small and the study was forgotten because it failed to prevent spinal cord injury in a subsequent study which was unfair because that was a totally different scenario.
However, history is now repeating itself with the finding that steroids might prevent PTSD:
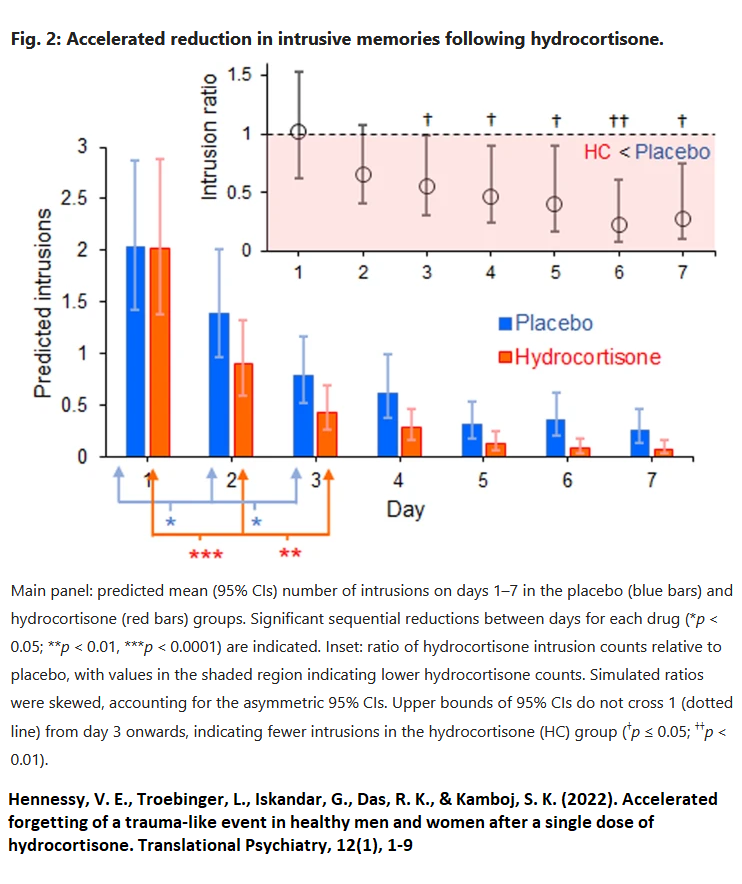
Hennessy, V. E., Troebinger, L., Iskandar, G., Das, R. K., & Kamboj, S. K. (2022). Accelerated forgetting of a trauma-like event in healthy men and women after a single dose of hydrocortisone.
Translational Psychiatry, 12(1), 1-9. (2022)
https://www.nature.com/articles/s41398-022-02126-2
- Watched a stressful film and chronologed number of recollections (memory intrusions)
- Hydrocortisone 30 mg (equivalent of prednisone 7.5 mg) after viewing
Results:
 Comment – if chronic pain is in part a pain memory, then steroid use early might prevent its formulation. Methylprednisolone has fallen out of favor as was often used as a pulse in Rheumatic conditions. What has been used instead was decadron high dose.
Comment – if chronic pain is in part a pain memory, then steroid use early might prevent its formulation. Methylprednisolone has fallen out of favor as was often used as a pulse in Rheumatic conditions. What has been used instead was decadron high dose.
Molenaar, D. S., P. A. Van Doorn, and M. Vermeulen.
Pulsed high dose dexamethasone treatment in chronic inflammatory demyelinating polyneuropathy: a pilot study.
Journal of Neurology, Neurosurgery & Psychiatry 62.4 (1997): 388-390.
https://jnnp.bmj.com/content/jnnp/62/4/388.full.pdf
- They used 40 mg orally a day for 4 days every 4 weeks – I gave dexamethasone 4 mg – 4 am, 3 afternoon, 3 evening = 10/day.
- Perhaps 1-2 days of it would be sufficient…
Comment – I feel strongly this is important and would have given that to patients early after a whiplash and maybe a PTSD experience.
Another drug with brain altering effects, and a propensity for some memory lose with, is ketamine. I had one lady with Multiple Sclerosis neurogenic pains and non-radiologic axial spinoarthropathy have a rollover while visiting her young son in Edmonton with advanced cancer. She uses ketamine at home (but not using it while driving :) ) as per my protocol:
Office Ketamine For Chronic Pain Poster
http://painmuse.org/?p=5611
she suffered no whiplash nor PTSD following which was amazing considering the stress she was under with her son ill. That should be assessed as well though a bad reaction to ketamine could aggravate PTSD so need to be careful…
