There can be a significant depression issue in chronic pain in which, if you scratch the surface, you find significant underlying anger is actually the issue. Inability to deal with the anger leads to significant depression and self-flagellation and increase suffering. I attempt to suggest to patient to say out loud “I forgive you” in regards to others but finds subjects choke up on that. Now it look like a way in, is to do loving kindness meditation (Tong Len taking and giving). This involves meditation plus imagining breathing in the black “pain” of others while breathing out an aura of happiness to others. My feeling is that doing that to ones you hate could help the issue and give you a sense of relief.
Carson, James W., et al.
Loving-kindness meditation for chronic low back pain: Results from a pilot trial.
Journal of Holistic Nursing 23.3 (2005): 287-304.
https://www.academia.edu/download/40338177/Loving-Kindness_Meditation_for_Chronic_L20151124-17210-1qijroj.pdf
- “Anger and resentment (e.g., toward self, spouse, health care providers, persons blamed for accidents leading to pain) appear to be salient features of many persons’ chronic pain experience”
- “The growing recognition that unchecked anger and resentment can complicate the treatment of persistent pain”
- 43 cases chronic back pain randomized to control of active group
- 8 weekly 90-minute group sessions
- daily practice of loving-kindness meditation
Procedure verbatum:
(a) recalling a time when they felt a very positive feeling of connection with a loved
one,
(b) letting go of the content of this memory while remaining focused on the actual feelings of love and kindness elicited in the present moment by the memory (this affective focus is distinct from the cognitive focus more typical of loving-kindness practice; e.g.,
Salzberg, 1995),
(c) employing silent mental phrases to direct these positive feelings, as best as possible, toward the loved one (i.e., may this person be at ease/content/happy/safe and secure) and then toward oneself, and
(d) during the final minutes of the meditation, patients were asked to rest with attention to any feeling of love that remained from the practice.
- After few weeks, process extended to “include directing positive feelings toward a
neutral person (e.g., postman, store clerk) - Subsequently “toward a person who harmed the patient or was a source of difficulty for them in the past in some way, and who they felt they could forgive to some extent (e.g.,
disrespectful former boss, dismissive former health care provider; perpetrators of sexual or physical abuse were explicitly excluded); - last Tong Leng toward all living beings
- They used progressive muscular relaxation – going through each part of your body and relaxing it in turn – called a body scan
- They felt “encourages patients to accept their bodies as they are and feel gratitude for what their bodies have enabled them to accomplish in life” – I don’t know – that might be a hard sell
Group practice:
- group exercises (e.g., consideration of forgiveness as a gradual process that
does not necessarily require any further contact with the offender but
rather is done to release oneself from the grip of anger and resentment
that has continued to affect one’s well-being), - group discussions (e.g.,experiences of practicing loving-kindness meditation and applying it to their daily lives),
- I have taking a course from Dr. Jackie Gardner-Nix (The Mindfulness Solution to Pain: Step-by-Step Techniques for Chronic Pain Management) and was impressed by the advantages of group sessions. They are put in groups of four around a table and get to know each other and are accepted. They interact and gain friendships. They each pick a handle for themselves which gives them some autonomy and identity.
Home therapy:
- “daily practicing audiotape-guided of loving-kindness strategies.
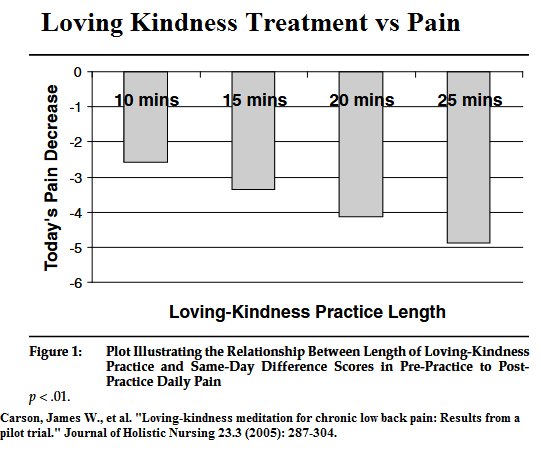
- do 10-30 minutes daily
Results:
Comment:
Looks like 25 minutes of practice could give significant help. When training in mindfulness mediation for pain, I felt a golden opportunity to offer positive suggestions could have been promoted. The mere presence of the program suggested it would work but there are now strategies to offer cognitive-behavioural advice during hypnosis-like sessions (mindfulness-based cognitive therapy) . Bipolar patients are represented in fibromyalgia victims and these cases can go hypomanic during sessions and need to be warned and monitored. I had one case that came back to bite me…