Do you have any further info up to date for 2010 as my IC friend’s condition is very severe presently for last 2 weeks & here in India we are being told they know little about IC. She’s desperate for some effective help asap. She’s history of 2 ulcers + suffers from gastritis & IC symptoms began to appear after her hip fracture with poor catheter asepsis was given. This whole bacterial over growth is something we would like to hear more in depth information about. Thank you.
This is tough – she needs a good workup first.
1) First of all your patient needs a workup of her condition:
– does she have fibroids pressing on her bladder giving her symptoms? An Ultrasound could find that – if not a pelvic exam.
– does she actually empty her bladder or does she get overflow incontinence? – Fullness suprapubic or an ultrasound or a post void catheterization could tell that.
– does she still have continued infections that are resistant to most antibiotics? Hopefully a urine culture could tell that. There is a school of thought that mild chronic infection exists, and if this so called Interstitial cystitis is new in an elderly subject one would wonder if there is continued infection. in:
Journal of Urology volume 172, Issue 1, Pages 232-235 (July 2004)
URINARY URGENCY AND FREQUENCY, AND CHRONIC URETHRAL AND/OR PELVIC PAIN IN FEMALES. CAN DOXYCYCLINE HELP?
FIONA C. BURKHARD, NADJA BLICK, WERNER W. HOCHREITER, URS E. STUDER
abstract here
They took cases of new frequency pain without cause and put them on Doxycycline 100 mg twice daily for two weeks – not hard to get – is a tetracycline used in malaria prevention sometime – must be taken with foo to prevent food tube erosions and might have to be taken with the cimetidine 400 mg twice daily to be tolerable. 70% got better. It was the authors feeling that IC should not be diagnosed without first trying this agent.
– Is she on water pills that could worsen her situation? – too much tea and coffee too
– does she have bladder cancer? – and where you are bladder TB?
– Is she able to concentrate urine or does she put out vast amounts of dilute urine (Diabetes insipidus).- Have her not drink one evening and see if her urine is concentrated the next day.
– Is she sugar diabetic? – a test strip might show sugor or better yet blood testing
-urinary frequency is common in Multiple Sclerosis – does she have neurological or previous eye symptoms?
– Is she malnutritioned? – supplements would help
_ Did she have a head injury with her hip fracture – are we dealing with a post- concussion syndrome as well.
– Is she depressed – this is common in IC and is a separate issue that needs treatment. In the elderly that con’t tolerate anything, DHEA is a herbal that can help at 100 mg 3 times daily – often very low in the elderly
Postmenopausal women have bladder problems because they are hypoestogenic – vaginal estrogen – premarin vaginal cream daily would help that.
2) There are some very simple measures that help IC:
Diet – a diet low in oxalates and irritants helps –
see IC association discussion here
CitroCal – one tablet with each meal cuts down urine oxalate excretion in urine and may help
H2 Blockers
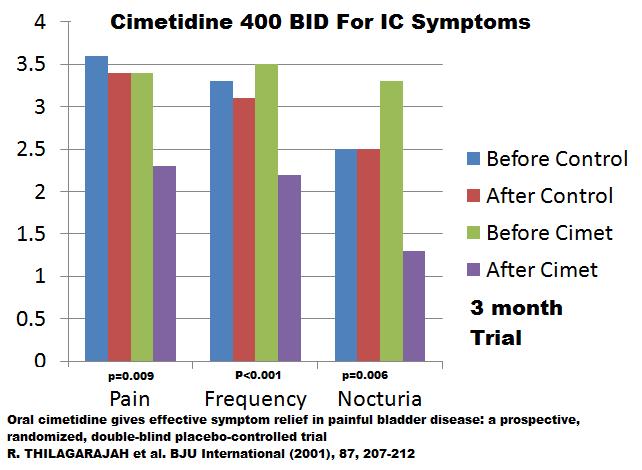
Tagamet – Cimetidine is available over the counter in many countries and found helpful in IC (used for stomach ulcers too!) 400 mg twice daily was helpful in IC:
BJU Int. 2001 Feb;87(3):207-12.
Oral cimetidine gives effective symptom relief in painful bladder disease: a prospective, randomized, double-blind placebo-controlled trial.
Thilagarajah R, Witherow RO, Walker MM. article here
H1 Antihistamines are helpful too:
Urology Volume 49, Issue 5, Supplement 1, Pages 108-110 (May 1997)
Hydroxyzine therapy for interstitial cystitis
Theoharis C. Theoharides, Grannum R. Sant
Start 25 mg hs 1st week, 50 mg hs second week, then 50 mg bed and 25 mg mid-day resulted in a 40% symptom reduction symptoms – but will cause drowsiness
Amitriptyline
Another valuable and inexpensive agent would be Amitriptyline – has antispasmodic(anticholinergic) properties, helps sleep, and stimulates brains own endorphins.
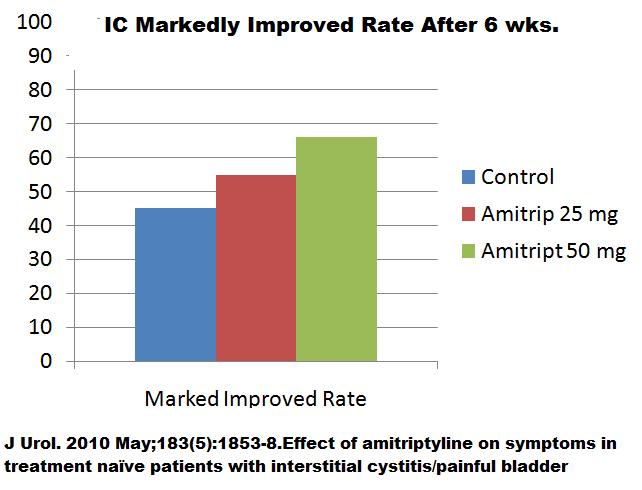
Urol. 2010 May;183(5):1853-8. Epub 2010 Mar 29.
Effect of amitriptyline on symptoms in treatment naïve patients with interstitial cystitis/painful bladder syndrome.
Foster HE Jr, Hanno PM, Nickel JC, Payne CK, Mayer RD, Burks DA, Yang CC, Chai TC, Kreder KJ, Peters KM, Lukacz ES, FitzGerald MP, Cen L, Landis JR, Propert KJ, Yang W, Kusek JW, Nyberg LM
abstract here
10 – 50 mg at bedtime helps IC but can really drug one at the higer dose – especially in elderly
Imipramine has been used as well:
Nishijima S, Sugaya K, Yamada T, Miyazato M, Ogawa Y (2006)
Efficacy of tricyclic antidepressants is associated with adrenoceptor genotype in patients with interstitial cystitis.
Biomed Res 27(4):163–167 free article here
They found 16% responded well, 29% fair, and the rest not at all.
More Advanced Treatments:
- Montelukast (Singulair) 10 mg daily
after 3 months – “urinary frequency had decreased from 17.4 to 12 voidings (p = 0.009), nocturia had decreased from 4.5 to 2.8 (p = 0.019) and pain had decreased from 46.8 to 19.6 mm
I had tried using it twice daily in selected cases as that is a dose that helps migraines - Gabapentin:
Sasaki K, Smith CP, Chuang YC, Lee JY, Kim JC, Chancellor MB
Oral gabapentin (neurontin) treatment of refractory genitourinary tract pain. Tech Urol 7(1):47–49, (2001) abstract here
worked up to a mean dose of 1200 mg – range 300 -2100. – These are mediocre doses though drowsiness and dizziness is an issue – they had 5/8 IC cases improved pain-wise. - Oral pentosan polysulfate sodium
Chuang YC, Lee WC, Chiang PH (2009)
Intravesical liposome versus oral pentosan polysulfate sodium for interstitial cystitis/painful bladder syndrome.
J Urol 182(4):1393–1400
100 mg three times a day – results for the price seemed rather mediocre
Pain scores at 8 weeks almost reached significance (p=0.054) though frequency was some better (p=0.019). - Alkalinized Lidocaine Bladder infusions: This seemed exciting and I wrote about it here:
Intra-Bladder Lidocaine Freezing to Diagnose Bladder Pain Syndromes and Lidocaine Treatments for Bladder Pain - Pelvic Floor Massage:
Part of the peripheral inflammation is stored in the muscles, and massaging them out can result in considerable benefits should the pelvic floor muscles be a player:
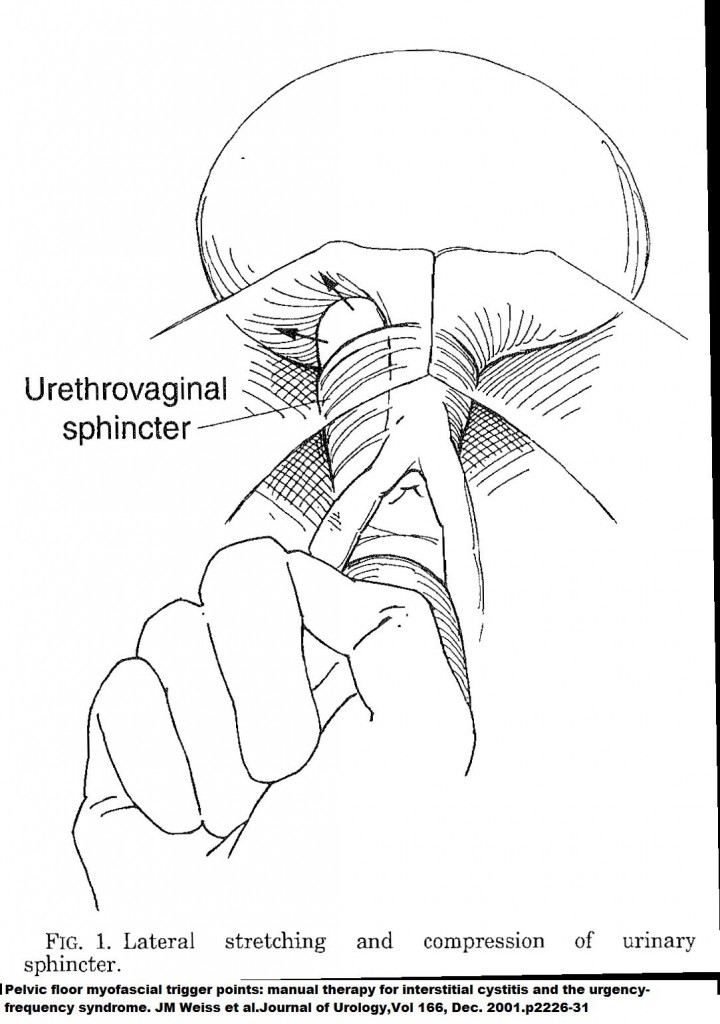
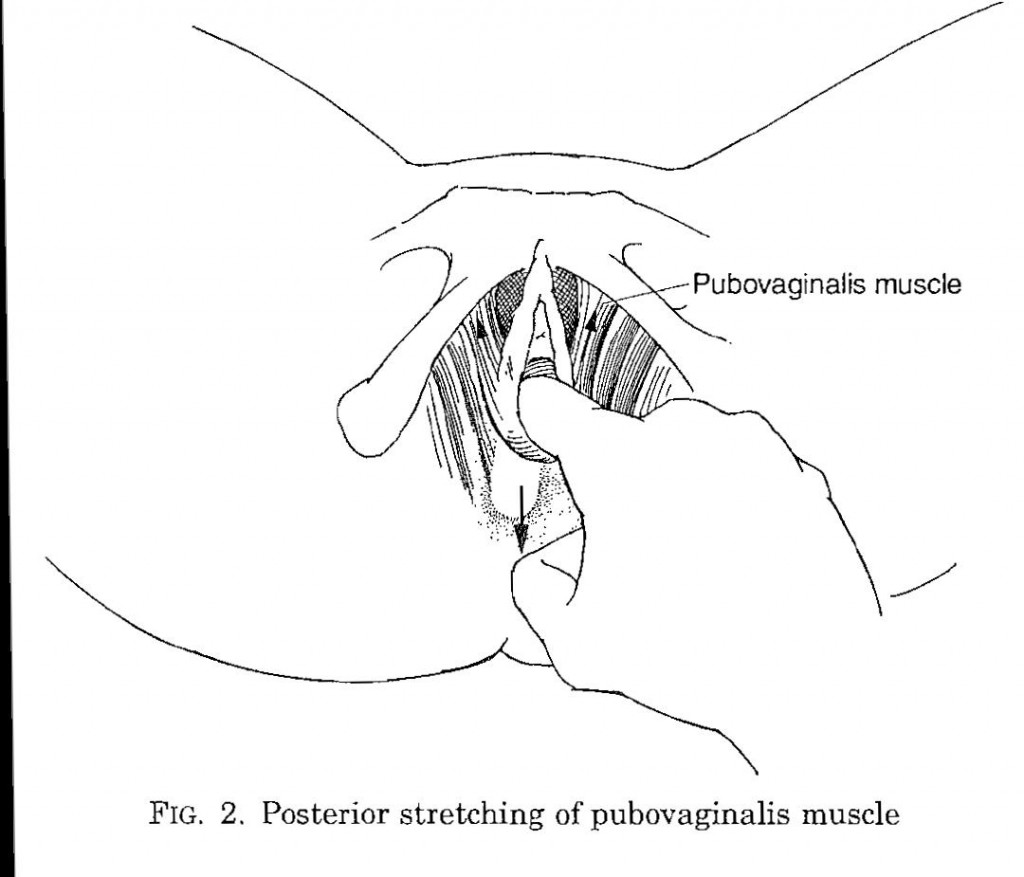
Pelvic floor myofascial trigger points: manual therapy for interstitial cystitis and the urgency-frequency syndrome
JM Weiss et al
Journal of Urology,Vol 166, Dec. 2001.p2226-31 free article here
The prime massage point is about the urinary sphincter as per diagram . Exact test description below:
1-2 visits weekly for 8-12 weeks
70% were moderate to markedly improved. –
Haven’t had much experience with it.
There are many other more complex and expensive treatments not mentioned here
What is getting more and more attention now is sacral stimulation – easier to put in then a pacemaker and fairly successful at symptom relief – I will go over that in another blog note sometime…
As for the bacterial overgrowth and IC, I had wrote about it here:
Restless Legs and Interstitial Cystitis Related to Gut Bacterial Overgrowth?
Where I discussed:
Small intestinal bacterial overgrowth in patients with interstitial cystitis and gastrointestinal symptoms
LB Weinstock, CG Klutke, HC Lin –
Digestive diseases and sciences, 2008 free article here
As for citations, there is one from the original author talking about restless legs:
Antibiotic therapy may improve idiopathic restless legs syndrome: Prospective, open-label pilot study of rifaximin, a nonsystemic antibiotic
Weinstock LB
SLEEP MEDICINE Volume: 11 Issue: 4 Pages: 427-427
and hence here
Dig Dis Sci. 2008 May;53(5):1252-6. Epub 2007 Oct 13.
Restless legs syndrome in patients with irritable bowel syndrome: response to small intestinal bacterial overgrowth therapy.
Weinstock LB, Fern SE, Duntley SP. abstract here
So can’t say how well it works . This drug is yet to be available in Canada so I haven’t tried it.
There are some bladder instillation treatments – DMSO, and hyaluronate
For patient involved – Sorry about your problems and good luck.. Let me know if any of this helps!



UTIs can be miserable for IC patients, and as you point out, that needs to be resolved.
I hope I can add some helpful information about IC treatment. I’m not sure if the ulcers the writer is referring to are gastric ulcers or Hunner’s ulcers in the bladder. Those can be treated with fulguration, laser ablation, or triamcinolone injection into the lesions. In May, the American Urological Association unveiled its preliminary clinical guidelines for IC, which should be helfpul. The ICA reported extensively on these in the Summer 2010 issue of the ICA Update, available through http://www.ichelp.org. You can also view a short presentation on the AUA webcast http://webcasts.prous.com/AUA2010/html/1-en/template.aspx?section=7&p=7,11883.
For immediate relief of bladder pain, instillations of anesthetics can be very helpful (http://www.ichelp.org/Document.Doc?id=20). Many of the treatments you mentioned can be very helpful as first- or second-line treatments. It seems as though this patient may have more severe disease, maybe enough to need third- or fourth-line treatments, as outlined in the new, preliminary guidelines. (The final guidelines should be issued by the end of the year.)
You might also find this review in Pain Practitioner helpful: http://www.aapainmanage.org/education/EducationLit/Pain%20Practitioner%20Spring_2010.pdf