Fibromyalgia posters at the IASP congress in Montreal highlighted abnormalities in DHEA and tryptophan. Treatments of these conditions could help. Testosterone could be a concern as well.
Tryptophan
PLASMA TRYPTOPHAN LEVELS ARE RELATED TO DEPRESSIVE SYMPTOMS AND TO THERMAL HYPERALGESIA IN MAJOR DEPRESSIVE DISORDER AND FIBROMYALGIA
IASP Poster Presentation Number: PT 226, Montreal 2010
- Low serotonin levels haave been related to both major depression and fibromyalgia
- Tryptophan is a precursor of serotonin
- It’s levels are low in both depression and FM
- their conclusion – “tryptophan could be involved in the pathophysiology of both disorders”
There are 2 studies using a tryptophan metabolite – 5-hydroxy-L-tryptophan:
J Int Med Res. 1992 Apr;20(2):182-9.
Primary fibromyalgia syndrome and 5-hydroxy-L-tryptophan: a 90-day open study.
Sarzi Puttini P, Caruso I.
J Int Med Res. 1990 May-Jun;18(3):201-9. abstract here
- “When all the clinical variables studied throughout the trial (number of tender points, anxiety, pain intensity, quality of sleep, fatigue) were compared with baseline results, they all showed a significant improvement (P less than 0.001). “
- “The overall evaluation of the patient condition assessed by the patient and the investigator indicated a ‘good’ or ‘fair’ clinical improvement in nearly 50% of the patients during the treatment.”
also:
primary fibromyalgia syndrome.
Caruso I, Sarzi Puttini P, Cazzola M, Azzolini V. abstract here
- good study – double blind
- 100 mg 3 times daily
- significant improvement in pain Visual Analog scale (VAS) and tender point counts
————————————————————– Next Poster is related to DHEA:
IASP Poster Presentation Number: PM 089, Montreal 2010
PERIPHERAL DHEA-S LEVELS ARE DECREASED IN FIBROMYALGIA AND NEGATIVELY CORRELATED WITH THERMAL HYPERALGESIA
M. Coulombe1, S. Potvin1,2, É. Paul-Savoie1, J. Corbin3, S. Marchand1
(DHEA is an adrenal hormone that counterbalances the detrimental effects of cortisol. It decreases as one gets older.)
- Low DHEA levels were found in both major mood disorder and Fibromyalgia, and the lower they were, the more heat sensitive the were found to be.
Various studies have demonstrated beneficial effects from DHEA:
Am J Psychiatry 156:646-649, April 1999
Double-Blind Treatment of Major Depression With Dehydroepiandrosterone
Owen M. Wolkowitz, M.D., Victor I. Reus, M.D., Audrey Keebler, B.A., Nicola Nelson, B.A., Mirit Friedland, B.A., Louann Brizendine, M.D., and Eugene Roberts, free article here
- 30 mg three times daily
“Five of the 11 patients treated with DHEA, compared with none of the 11 given placebo, showed a 50% decrease or greater in depressive symptoms.”Arch Gen Psychiatry. 2005;62:154-162
Dehydroepiandrosterone Monotherapy in Midlife-Onset Major and Minor Depression
Peter J. Schmidt, MD; Robert C. Daly, MD; Miki Bloch, MD; Mark J. Smith, MD, PhD; Merry A. Danaceau, RN; Linda Simpson St. Clair, RN; Jean H. Murphy, RN, MSN; Nazli Haq, MA; David R. Rubinow, MD free article here- tried 2 doses 30 mg and 150 mg three times daily
- Could not conclude if one dose was better but did get improvement compared to placebo:
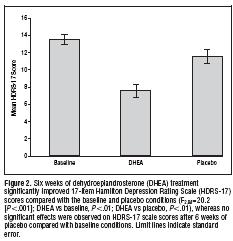
As you can see, DHEA cut depression scores in nearly half.
What about in FM?
The Journal of Rheumatology July 1, 2005 vol. 32 no. 7 1336-1340
A Randomized Controlled Trial of Dehydroepiandrosterone in Postmenopausal Women with Fibromyalgia
AXEL FINCKH, ISABELLE CAREY BERNER, BÉRENGÈRE AUBRY-ROZIER, and ALEXANDER KAI-LIK SOthey used 50 mg ONCE daily and observed no effect on Fibromyalgia
Gd’ help me – another MORON study which appears so good because it is randomized and controlled.
There was a study on MS sufferer taking DHEA:
Evaluation of DHEA Levels in Multiple Sclerosis by Subhuti Dharmananda
at: http://www.itmonline.org/arts/dhea.htmthey wrote about what happened to DHEA levels with once daily dosing:
“One patient did not take her morning dose of DHEA for the two days prior to the test. Her DHEA level at the second test was almost identical to the baseline level (32.9 mg/dl versus 32.6 mg/dl for the second test), indicating that the orally consumed DHEA was completely removed by that time. Further, there was no evidence of decline in her usual DHEA production level as a result of six weeks of daily ingestion of 15 mg. “
so DHEA level can return to baseline with once daily use.
The J of R article claimed the DHEA levels had tripled but I’m thinking they took levels within some hours of taking their once daily DHEA – probably wasn’t tripled by the morning…
Therapeutic dosing has been 30 mg THREE times daily and they stick to a punny 50 mg once a day – what a disappointing waste of time… So doing not much they achieved not much. How do I know? – They reported no improvement in depression when we know from good studies that with adequate dosing it should cut depression in nearly half…
When I use DHEA in depression treatment I use 100 mg TID – I do not believe that “normal” blood levels will bring about relief – I suspect it would take supernormal levels – I use 100 mg three times daily – it is a steroid hormone so I do breast exams for lumps just in case..
Why do you need supranormal levels? because some of it gets converted to testosterone – which takes us to the third problem discussed after this one.
Fibromyalgia subjects have more depressive tendencies – with good reason because this disorder can be quite painful. About 1/3 of victims have chemical sensitivites – perhaps related to its association with mast cell diseases.
Some cannot tolerate any antidepressants – they can however take DHEA because the effects are not serotonergic. If higher DHEA levels associated with less pain senstivity hyperalgesia then perhaps their pain could get some better to – no guarentees about latter though.
Where do you get DHEA? – from ebay but it is better that you make the dilevery point a doctor’s office – otherwise it might not make it into Canada – in US, you can get over the counter.
———————————
Testosterone (Androgens) – both men and women make testosterone and it determines sex drive for both. I routinely do androgen levels in women with chronic pain and find most often the are unmeasurable.
in:
Dessein PH, Shipton EA, Joffe BI, Hadebe DP, Stanwix AE, Van der Merwe BA:
Hyposecretion of adrenal androgens and the relation of serum adrenal steroids, serotonin and insulin-like growth factor-1 to clinical features in women with fibromyalgia.
Pain 1999, 83:313-319.They found BOTH DHEA levels and Androgen levels were “markedly decreased” as observed by:
Psychological stress and fibromyalgia: a review of the evidence suggesting a neuroendocrine link
Anindya Gupta and Alan J Silman
Arthritis Res Ther 2004, 6:98-106 free article here
They go further and say:“There is indirect evidence that fibromyalgia may be a consequence of low androgens. Fibromyalgia has many anti-anabolic features, such as muscle pain and fatigue, typically seen in androgen-deficiency states. Androgens exert anabolic effects, particularly on muscle. They promote muscle growth and healing, and androgens have been used for this purpose after trauma, after prolonged immobilisation and in individuals with debilitating illness [60]. However, no therapeutic trials of androgens have been conducted in fibromyalgia.”
Why would women end up with low androgens? – it’s very simple actually – people with sleep apnea end up with low androgens and women with FM often have sleep disordered breathing. Interestingly this condition occurs with menopause as well:
J Clin Sleep Med. 2005 Jul 15;1(3):291-300.
Menopause related sleep disorders
Eichling PS, Sahni J.
In the article, they discuss the link with FM:“Sleep disordered breathing (SDB) increases markedly at menopause for reasons that include both weight gain and unclear hormonal mechanisms. Due to the general under-recognition of SDB, health care providers should not assume sleep complaints are due to vasomotor related insomnia/depression without considering SDB. Fibromyalgia has gender, age and probably hormonal associations. Sleep complaints are almost universal in FM. There are associated polysomnogram (PSG) findings. FM patients have increased central nervous system levels of the nociceptive neuropeptide substance P (SP) and lower serotonin levels resulting in a lower pain threshold to normal stimuli. High SP and low serotonin have significant potential to affect sleep and mood. Treatment of sleep itself seems to improve, if not resolve FM. Menopausal sleep disruption can exacerbate other pre-existing sleep disorders including RLS and circadian disorders. ”
Use of opioids is also associated with low androgens levels. – It gets worser and worser..
I check testosterone level and treat accordingly. The most effective treatment is Testim gel 0.2-0.3 mls/day put on a forearm. I had one lady who wanted a bio-identical testosterone – as soon as she found out from a friend how much the testim had helped energy etc., she came in and wanted to be switched to the testim…
- Androgens can build bone and muscle – something postmenopausal women could use – at doses used should not make masculine,
- Other issues not mentioned include Thyroid, vitamin D and B12 levels.