In those patients with Irritable bowel and restless leg syndrome, significant benefits can occur if therapy to treat bacterial overgrowth is undertaken
1) Previous studies have suggested a high proportion of Irritable bowel patients have evidence of bacterila overgrowth and their symptoms respond to certain antibiotics.
World J Gastroenterol. 2007 Dec 7;13(45):6016-21.
Breath test for differential diagnosis between small intestinal bacterial overgrowth and irritable bowel disease: An observation on non-absorbable antibiotics.
Esposito I et al
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4250883/
2) About 45% have evidence of Bacterial overgrowth and many of those respond well to rifaximin 1200 mg/d for seven days. This antibiotic is not available in Canada yet so another study found Neomycin 500 mg BID could be used. I had the pharmacy order in some powder. 500 mg of powder is measured out and put in a container as an example. The patient is to consume roughly that BID for a week. If there is any concern re Neomycin allergy, have them tape some of the powder to the forearm for a few days and see if there is a reaction. In the Rifaximin study, the few who did not get better were given courses of Ciprofloxin 500 mg BID for 7 days.
Degree of bacterial overgrowth is measured by the amount of laculose (an non-absorbed sugar)
Test would be similar to this:
3) Restless Leg Connection: – Using similar treatment “Ten of 13 patients exhibited >/=80% improvement from baseline in RLS symptoms. Five maintained complete resolution of RLS symptoms. “
Weinstock, Leonard B., Steve E. Fern, and Stephen P. Duntley.
Restless legs syndrome in patients with irritable bowel syndrome: response to small intestinal bacterial overgrowth therapy.
Digestive diseases and sciences 53 (2008): 1252-1256.
https://citeseerx.ist.psu.edu/document?repid=rep1&type=pdf&doi=48b2ec6b5975ebfd22c30991fe5398efa15574ba
“patients with abnormal lactulose breath tests received rifaximin 1,200 mg day –1
for 10 days, followed by tegaserod 3 mg, long-term [pulled from market], and
1 month of zinc 220 mg day –1 and once-daily probiotic (N = 11) or rifaximin monotherapy (N = 2).”
“Results Ten of 13 patients exhibited >/=80% improvement from baseline in RLS symptoms. Five maintained complete resolution of RLS symptoms.”
4) Interstitial Cystitis Connection: Even more shocking is the fact some Interstitial cystitis may respond to the same:
Lin, Henry C.
Small Intestinal Bacterial Overgrowth in Patients with Interstitial Cystitis and Gastrointestinal Symptoms.
Dig Dis Sci 53 (2008): 1246-1251.
https://www.researchgate.net/profile/Leonard-Weinstock/publication/5911997_Small_Intestinal_Bacterial_Overgrowth_in_Patients_with_Interstitial_Cystitis_and_Gastrointestinal_Symptoms/links/0deec53b4035ea1779000000/Small-Intestinal-Bacterial-Overgrowth-in-Patients-with-Interstitial-Cystitis-and-Gastrointestinal-Symptoms.pdf
Purpose Interstitial cystitis (IC) often coexists with irritable bowel syndrome (IBS). IBS may be explained by small-intestinal bacterial overgrowth (SIBO), which increases immune activation and visceral hypersensitivity. This prospective pilot study tested hypotheses that IC patients with gastrointestinal (GI) symptoms have SIBO, that nonabsorbable antibiotic use improves symptoms, and that
improvement is sustained by prokinetic therapy. Methods Consecutive IC patients with GI symptoms had lactulose breath testing (LBT). Those with abnormal results received rifaximin 1,200-1,800 mg/day for 10 days then tegaserod 3 mg/nightly. Questionnaires addressed IC and GI global improvement. Results Of 21 patients, 17 (81%) had abnormal LBTs. Of 15 patients treated, GI global improvement was moderate to great in 11 (73%) and sustained in ten (67%). IC global improvement was moderate to great in six (40%) and sustained in seven (47%). Conclusions A majority of IC patients and GI symptoms had an abnormal LBT suggesting SIBO.
Rifaximin improved symptoms, which was sustained by tegaserod.
Wow – what a paradigm shift – Irritable bowel, restless legs and Interstitial Cystitis are in part bacterial overgrowth syndromes .
The link between FM and irritable bowel might relate to this bacterial overgrowth:
Ann Rheum Dis 2004;63:450–452.
A link between irritable bowel syndrome and fibromyalgia may be related to findings on lactulose breath testing
M Pimentel, D Wallace, D Hallegua, E Chow, Y Kong, S Park, H C Lin article here
Fibromyalgia may temporarily respond to treatment of bacterial overgrowth as described by this patent:
Method of diagnosing fibromyalgia caused by small intestinal bacterial overgrowth
Patent US 7056686 B2
H.Lin et al
http://www.google.com/patents/US7056686
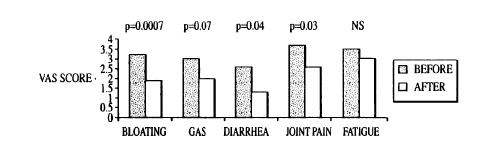
(FM/IBS symptoms after Neomycin 500 mg twice daily X 10 days.)
Another treatment for Irritable bowel is the use of Probiotics. Tu Zen (Ferring pharmaceutics) Lactobacillus given two a day. It comes in a $40.00/ 30 pill boxes. If there is a response after two weeks, they suggest 6 weeks therapy for optimum results. Relief is maybe 30-40% at 6 month followup. Shoppers South Albert Landmark in Regina carries it in the pharmacy (have to ask for it). It is a live culture – it cannot go in freezer and it does not like temperatures over 20 degree C. (72 degree F.) – so maybe keep in fridge.
Ferring also sells BioGaia® Lactobacillus DROPS for baby colic. It reduced crying from 3.2 hours initially to 0.85 hour after 28 days.
abstract here full article
Simethicone drops control group went from 3 to 2.4 hours after 28 days. Have used it and found moms not surprisingly grateful.
Now things get more complex. There seems to be a subgroup of people with Irritable bowels that have subclinical microscopic colitis or “marginal” celiac – ie. a recent study found among the diarrhea based Irritable bowel subjects, half will clear off gluten at 6 month followup despite celiac antibodies in the normal range (were higher normal than non-responders though). These bowel groups can have coexistant mild spondylitis (back inflamed). Conversely, people with ankylosing spondylitis can demonstrate occult colitis as a symptom.
Point being?
Probiotics may reduce the spondylitis symptoms in these cases as suggested below>
article here
Any comments?

I found your blog via Google while searching for mail order antibiotics and your post regarding Restless Legs and Interstitial Cystitis Related to Gut Bacterial Overgrowth? looks very interesting to me. Just wanted to drop you a quick note to say thank you for a great resource.There is nothing else like your site on the net today. My friends are just going to love this site once I let them know about it.
Pingback: Pain Medical Musing » Blog Archive » Bacterial Overgrowth causing Chronic Pancreatitis and Rosacea - New treatment? And, for elderly, a quick way to get rid of lactose intolerance
One friend has IC and another has restless leg syndrome. This info on your site has thrown a different view on possible treatment options not thought of before. Thank you. Would appreciate latest updates on this from you as this is 2007 publication as both these friends have not been receiving adequate or effective treatment.
Hi, weird. I also had IC with RLS. Used probiotics and helped the IBS and RLS. Went for cystoscopy and dilation for IC and urologist says urether is still inflammed and gave antibiotics. I kept googling my symptoms and never thought there was a connection. Thanks for a very interesting article.
I have all RLS, IBS and was just diagnosed with IC. I decided to google all three to see if maybe there is a connection and I came across your site. Thank you!
I too have RLS along with I.C. Fibromyalgia, and Underactive Thyroid Disorder., and have also been treated for Helicobactor Pylori Infection. Can anyone tell me what the link between them all is.
I too have Restless Leg, I.C. and Hunners Ulcer, Fibromyalgia and an Underactive Thyroid. was treated twice for Helicobactor Pylori Infection., and Migraine. No medic will say they are related, I am taking Mirapixin for the Restless Leg Syndrome, Eltroxin for the Underactive Thyroid, Elmiron for I.C. And Amytriptline for Migraine. I wish someone to find the link between all of the above
I too have Restless Leg, I.C. and Hunners Ulcer, Fibromyalgia and an Underactive Thyroid. was treated twice for Helicobactor Pylori Infection., and Migraine. No medic will say they are related, I am taking Mirapixin for the Restless Leg Syndrome, Eltroxin for the Underactive Thyroid, Elmiron for I.C. And Amytriptline for Migraine. I wish someone to find the link between all of the above